In practice, posterior disc bulge is one of the most commonly misunderstood disc issues. A posterior disc bulge may be present for years without creating disc pain. Another posterior disc bulge may suddenly become clinically relevant because it is causing symptoms related to nerve irritation or reduced adaptability. The difference is not just the disc itself. It is how the spine, the spinal nerve system, and the nervous system as a whole are responding.
Chiropractors are uniquely positioned to lead this conversation. A posterior disc bulge is not a diagnosis by itself. It is an anatomical description that must be interpreted through function. When that interpretation is grounded in neurological scanning, objective exam data, and confident communication, the disc finding stops being a fear trigger and becomes a manageable part of a care plan.
Understanding the Posterior Disc Bulge Through a Chiropractic Lens
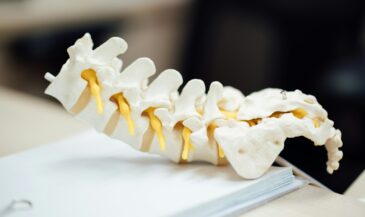
A posterior disc bulge refers to a spinal disc that extends beyond its usual boundary toward the back of the spine. The intervertebral disc sits between each vertebra and functions as a shock absorber. Disc anatomy includes the nucleus pulposus inside the disc and the annulus fibrosus forming the outer layer. When the disc extends beyond the vertebral margin, it is called a bulge. When that extension is directed toward the back of the disc, it is labeled posterior.
In a healthy spine and disc relationship, the outer edge of the disc generally aligns with the edge of the vertebra above and below. With disc degeneration and wear and tear, the disc may lose hydration and resilience. As pressure on the affected disc increases, the disc extends beyond its typical boundary. A posterior disc bulge describes the location of that extension, not its severity.
This distinction matters. A disc bulge may be small, broad-based, or asymmetric. A posterior disc bulge may involve a limited portion of the disc or a larger area. The disc may remain fully contained inside the disc, or it may be associated with additional disc pathology. Chiropractic interpretation begins by understanding that a posterior disc bulge is a structural finding that becomes clinically meaningful only when correlated with function.
The reason posterior location gets attention is proximity. The back of the disc is closer to the spinal canal, spinal nerve tissue, and the nerve root region. A posterior disc bulge may be entirely quiet, or it may contribute to irritation if the bulging disc presses into nearby space. The chiropractor’s role is not to overstate risk but to evaluate whether the disc is bulging in a way that affects neurological performance.
- A disc bulge describes contour, not damage.
- Posterior location increases the need for careful correlation.
- Function determines relevance, not imaging alone.
Posterior Disc Bulge vs Herniated Disc
The conversation around posterior disc bulge vs herniated disc is one of the most important educational moments in chiropractic care. A bulging disc and a herniated disc are often spoken about interchangeably, but they are not the same disc pathology. Understanding the difference helps chiropractors guide patients away from unnecessary fear.
A disc bulge occurs when the nucleus pulposus shifts outward but remains contained within the annulus fibrosus. The disc extends beyond the vertebral margin, but the outer layer is intact. Radiology may describe this as a broad-based disc, a diffuse disc bulge, an asymmetric disc bulge, or a circumferential disc bulge involving the entire disc. In many cases, a disc bulge generally reflects degenerative change rather than acute injury.
A herniated disc occurs when the annulus fibrosus is compromised. In this case, disc material may move beyond the normal containment. A herniated disc may be described as disc prolapse, disc protrusion, or disc extrusion depending on how far the disc material has moved. Herniated disc occurs when inner material escapes the outer layer and interacts with surrounding tissue.
Clinically, the difference matters because herniated disc pain and herniated disc symptoms become more likely when disc material contacts a nerve root or spinal nerve. In the lumbar spine, lumbar disc herniation may create leg referral. In the neck, a herniated cervical disc may create arm symptoms. A bulging disc may cause pain as well, but the mechanism is often pressure, inflammation, and reduced space rather than free disc material.
The key takeaway for chiropractors is this: a posterior disc bulge is not simply a mild version of a herniated disc. They are different processes. A bulging disc may never progress. A herniated disc may stabilize. Imaging describes shape, but neurological assessment explains impact.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Causes, Disc Degeneration, and Why Location Matters
Most posterior disc bulge findings are the result of cumulative stress rather than a single event. Disc degeneration develops over time as the disc loses hydration and elasticity. This wear and tear changes how load is distributed through the spine and disc system. As the disc weakens, the disc may extend beyond its normal boundary.
Common bulging disc causes include aging, repetitive strain, poor posture, improper lifting, prolonged sitting, ergonomic stress, prior injury, and genetic predisposition. A bulging disc happens when the disc is asked to tolerate more load than it can manage. Over time, disc issues develop as the disc adapts poorly to repeated stress.
Location of the bulge is critical. A posterior disc bulge extends toward the back of the disc where spinal nerve structures reside. In the lumbar spine, a posterior disc bulge may affect the traversing nerve root. In the cervical disc region, a posterior bulge may affect arm-related nerve pathways. The location of the bulge influences whether symptoms like numbness, weakness, or referral develop.
Chiropractors must also consider how the spine adapts globally. A posterior disc bulge often triggers protective muscle tension above and below the involved level. The body shifts movement strategies to reduce pressure on the affected disc. Over time, this compensation pattern may become more limiting than the disc finding itself.
Clinical Presentation, Symptoms, and Conservative Chiropractic Care
Many patients with a posterior disc bulge have no disc symptoms at all. A disc is bulging on imaging, yet function remains intact. When a posterior disc bulge is causing symptoms, it is often because the bulging disc presses into sensitive tissue or increases pressure on the affected disc.
Symptoms of a bulging disc may include localized back pain, stiffness, or reduced range of motion. Bulging disc symptoms may also include radiating sensations, numbness, tingling, or weakness when a nerve root is irritated. Symptoms like electrical sensations, heaviness, or sharp pain may appear. A disc bulge may cause pain intermittently depending on posture and activity.
Conservative chiropractic care is the primary treatment approach for most posterior disc bulge cases. Nonsurgical treatment focuses on restoring movement, reducing protective tension, and improving neurological function. Treatment options may include activity modification, adjustments, rehabilitation strategies, and disc bulge exercises designed to improve movement tolerance.
Bulging disc treatment does not mean chasing the disc. Treatment involves supporting the spine so the nervous system can adapt more effectively. A disc bulge treatment plan should be structured, progressive, and measured. Surgical treatment and spine surgery are typically reserved for persistent cases with progressive neurological compromise.
- Most disc bulge cases respond well to conservative care.
- Appropriate treatment focuses on function, not fear.
- Effective treatment is guided by objective findings.
Posterior Disc Bulge and the Role of INSiGHT Neurological Scanning
A posterior disc bulge becomes problematic when it is viewed in isolation. Imaging shows what the disc looks like, but it does not show how the nervous system is responding. This is where INSiGHT scanning changes the quality of care. Neurological scanning allows chiropractors to measure function rather than speculate.
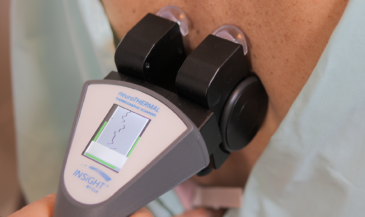
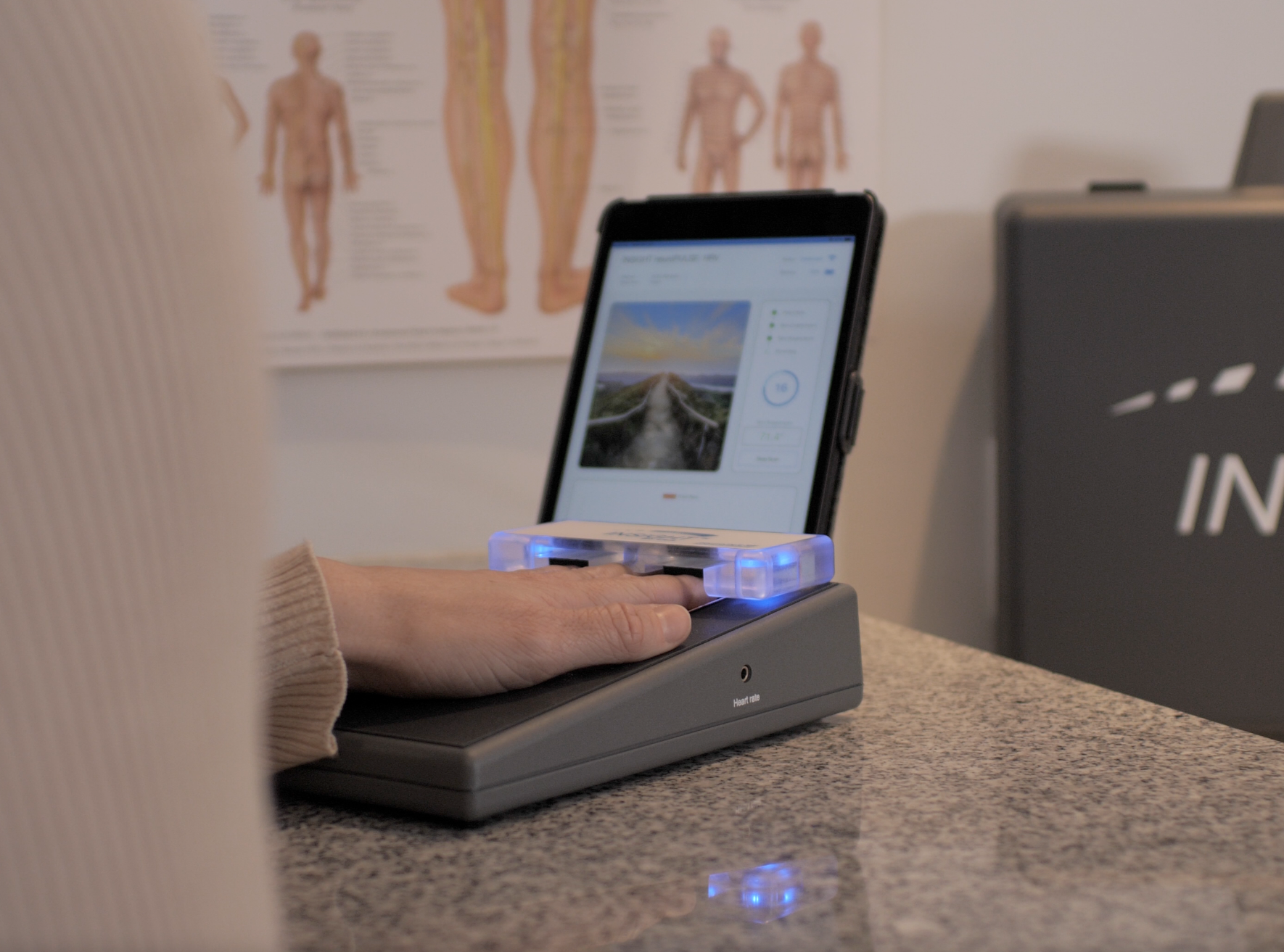
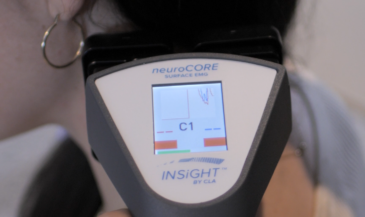
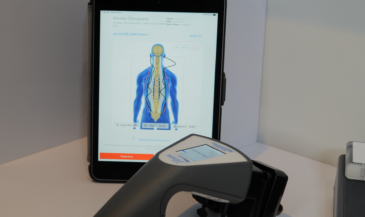
The neuroTHERMAL scan identifies segmental stress patterns along the spine, highlighting areas of dysregulation associated with disc pathology. The neuroCORE sEMG scan evaluates postural tension and motor compensation that often develops around a bulging disc presses scenario. The neuroPULSE HRV scan provides insight into adaptability and recovery, showing how well the nervous system is managing stress.
When chiropractors integrate INSiGHT scanning technology, the posterior disc bulge conversation shifts. Patients see objective scan views instead of imagining worst-case outcomes. The disc finding becomes one piece of the spine and disc story. Progress is tracked, certainty improves, and patients understand why care continues even when pain and other symptoms fluctuate.
From Disc Fear to Neurological Clarity
A posterior disc bulge does not have to define a patient’s future. It is a structural finding that must be interpreted through function. Chiropractors excel at connecting disc findings to nervous system performance. When that connection is supported by neurological scanning, the conversation becomes clearer and more grounded.
Instead of asking whether the disc is damaged, patients learn to ask how their nervous system is adapting. Instead of fearing movement, they build confidence. Instead of chasing labels, chiropractors lead with measurable progress. Posterior disc bulge becomes a starting point, not an endpoint, when clarity replaces fear.