Here is the problem with the usual conversation. When stress is treated like a vague emotional cloud, the story gets fuzzy. Patients feel dismissed. Chiropractors feel like they are guessing. And the care plan conversation turns into opinions instead of clarity. But when you recognize the neurological symptoms of stress for what they are, real outputs of a real stress response, the case becomes easier to explain and far easier to track.
Chronic stress is where things get loud. When the stress response keeps running, the body stays exposed to stress hormones and the nervous system starts acting like it is living in an emergency. Stress hormones like cortisol do what they are designed to do, they keep the system ready. But when this becomes chronic, the same chemistry that helped someone survive a moment can start to interfere with brain health, sleep, pain processing, and day-to-day function. That is why neurological symptoms of stress deserve a chiropractor’s attention, not as a side topic, but as a core part of the clinical conversation.
Stress Is a Neurological Event First, Then a Symptom Story
In a neurologically focused chiropractic practice, stress is not background noise. It is often the lens that makes the case history make sense. The stress response is a brain-led survival program. It is designed to activate quickly, prepare the body, and help us respond to a threat. That is not pathology. That is physiological reality. The challenge is that modern life rarely gives patients a clean “threat over, recovery on” moment. Stress persists, and the brain’s response to stress keeps running.
This is why the phrase neurological symptoms of stress is clinically useful. It tells the patient that what they are experiencing is not random or imaginary. It is a nervous system output. Stress affects the nervous system, and when the body stays on high alert, symptoms can show up in cognition, sensation, motor control, sleep, and emotional regulation. Chiropractors see patients repeatedly over time, which means you are in a unique position to spot persistent stress early, document it, and track change instead of guessing.
It also helps to separate acute stress from chronic stress. Acute stress is the short burst. It may sharpen attention, increase alertness, and give a temporary boost in energy. That is a normal response to stress. But long-term stress changes the tone of the system. When stress becomes chronic, the body stays exposed to levels of stress hormones that were never meant to be elevated all day, and the symptoms shift from “I feel keyed up” to “I feel like something is off.” That is where neurological symptoms of stress start to multiply.
- Acute stress: quick activation, short-lived, often followed by recovery.
- Chronic stress: ongoing activation, reduced recovery capacity, and stress-related complaints that compound over time.
At the center of this conversation are stress hormones, especially cortisol and adrenaline. The release of stress hormones is part of what allows the body to mobilize. Cortisol helps regulate energy availability. Adrenaline drives arousal and urgency. This is the “fight or flight” program doing its job. But when cortisol stays elevated, cortisol levels can become a marker of a system that cannot downshift. This is the stress affect you hear when a patient says, “I’m tired but wired.” And it is why managing stress is not a pep talk. It is a clinical strategy that supports nervous system functions.
The Brain Under Stress and the Neurological Mechanisms Behind Symptoms
Once you stop treating stress like a personality trait and start treating it like a neurological load, the whole case looks different. Stress affects the brain because the brain decides what is dangerous, what is urgent, and what deserves attention right now. Then it sends signals through neurology, through chemistry, and through the autonomic nervous system. In the short term, that is protective. In the long term, stress on the brain can become disruptive. This is where chiropractors can bring clarity without stepping outside scope. You are not diagnosing disease, you are explaining how stress affects the brain and why a patient’s symptoms can be a predictable output of a system stuck in high gear.
When chronic stress is present, the body experiences prolonged exposure to stress hormones like cortisol. Cortisol is not “bad,” but it is powerful. Over time, elevated cortisol levels can interfere with sleep quality, memory formation, attention, and emotional regulation. Patients call it brain fog. They describe forgetfulness, scattered thinking, and irritability they do not recognize in themselves. Research suggests that chronic stress is associated with measurable shifts in brain function, and suggests that chronic stress may be tied to changes in brain structure in key regions. In plain language, chronic stress impacts your brain in ways that make daily life feel heavier than it should.
The three regions that show up repeatedly in reputable summaries are the hippocampus, the prefrontal cortex, and the amygdala. The hippocampus plays a major role in memory and learning. Some sources describe that chronic stress may be associated with shrinkage in the hippocampus, which helps explain memory lapses and the mental fatigue that patients describe. The prefrontal cortex supports decision-making, attention regulation, and impulse control. When the prefrontal cortex is not running efficiently, the patient may feel reactive, scattered, and unable to focus even when they want to. The amygdala is the brain’s fear center, and chronic stress may increase its activity, creating a loop of heightened threat detection. In other words, a specific brain region can become biased toward danger, and the patient experiences that bias as anxiety, tension, and a body that never fully relaxes.
Bring that back to what you see in practice. The neurological impact of prolonged stress is that the system becomes easier to flare and harder to settle. Stress impairs recovery, and that changes how patients experience pain, sleep, mood, and sensation. Stress also disrupts sleep and recovery signals, which is why the effects of stress show up as headaches, fatigue, dizziness, and sensitivity that feels out of proportion. That is the relationship between stress and symptoms in real life, and it is why neurological symptoms of stress belong in your exam conversation.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Recognizing the Neurological Symptoms of Stress in Chiropractic Settings
Let’s make this practical. In the chiropractic industry, the stress conversation often shows up disguised as something else. A patient books for headaches. Or neck and shoulder tightness. Or low back tension that returns the second they leave the table. But if you slow down and listen, you will often hear the same thread: persistent stress, poor recovery, and a stress response that never turns off. Recognizing the signs early helps you build clarity without minimizing the patient.
One of the most common neurological symptoms of stress is cognitive dysfunction. Patients describe brain fog, poor concentration, difficulty processing information, and memory lapses that scare them. They might say, “I cannot think straight,” or “I feel like I have lost my edge.” This is where stress and brain health becomes a real conversation. Stress affects the brain systems tied to attention and memory, and chronic stress may show up as reduced mental flexibility and lower tolerance for stimulation. Chiropractors do not need to act like a neurologist to take this seriously. You just need to document it, connect it to the stress response, and track whether it improves as recovery improves.
Then come the physical complaints that sound musculoskeletal but often carry a stress-related layer underneath. Headaches are a big one, including tension headaches and migraines. Patients also report muscle pain, stiffness, and a guarded feeling in the neck and shoulders. Stress impacts pain processing, and the impact of stress can show up as increased sensitivity and longer recovery time. Chronic pain becomes part of the picture too, because pain can keep the stress response active, and stress can amplify pain. That is stress and neurological in a loop, not just in theory, but in day-to-day practice.
Watch for sensory complaints as well. Tingling, numbness, pins-and-needles sensations, and sensitivity to touch or temperature are all described as stress-related neurological symptoms. Patients may ask, “Can stress cause neuropathy?” Stress may contribute to how symptoms feel, and stress-related changes in inflammation, blood flow, and sensitivity can exacerbate existing issues, but stress is not typically a direct cause of neuropathy. If symptoms are persistent, progressive, or paired with weakness, coordination changes, or severe balance issues, collaboration matters. This is where you may recommend evaluation with a neurologist for expert neurological care. This keeps you honest, protects the patient, and strengthens trust.
Finally, look for the cluster that often travels together: motor and balance complaints, sleep disruption, and emotional reactivity. Tremors, muscle spasms, dizziness, vertigo, and unsteadiness are often reported due to stress, especially when stress persists. Sleep issues show up as insomnia, waking unrefreshed, or crushing fatigue. And emotional changes such as irritability, panic sensations, and heightened fear response can accompany these, especially when the amygdala stays on high alert. These are neurological symptoms of stress showing up across multiple systems, and they deserve a structured, measurable approach.
Why Chronic Stress Raises Risk and Complicates Outcomes Over Time
Stress is normal. The stress response is not the enemy. The problem is the impact of chronic stress. When stress becomes chronic, the body stays exposed to stress hormones, especially cortisol, and recovery becomes unreliable. This is where chronic stress impacts stop feeling like “a stressful season” and start showing up as a lasting shift in how the person functions. That includes mood, cognition, sleep, and pain modulation. In the clinic, you feel it as a patient who flares easily, heals slowly, and cannot maintain stability.
This is also where chiropractors can communicate risk in a grounded way. Chronic stress contributes to a higher likelihood of anxiety and depression, and it is commonly discussed alongside mood disorders and other mental health conditions. That does not mean stress automatically causes neurological disorders, but it does mean stress may increase the risk of longer-lasting complaints and reduced resilience when recovery never catches up. Research suggests that chronic stress can be associated with changes in key brain regions that support memory and emotional regulation, which connects directly to brain health and daily function. The impact of stress on neurological function is not abstract. It is measurable as reduced adaptability and slower recovery. That is one reason stress management belongs in the care conversation, even when the chief complaint is pain.
Let me say this clearly for chiropractors. This is not a fear tactic. It is clinical honesty. Chronic stress impacts your brain, and effects chronic stress can ripple through mental and physical health. Stress also disrupts sleep, and when sleep is not restorative, patients lose one of the biggest recovery advantages they have. This is where you encourage proactive steps to manage stress and help the patient manage stress effectively, because those steps support nervous system performance and consistency. When the picture looks bigger than functional stress, you refer appropriately. When it looks like stress-related dysregulation, you track it and guide it with clarity.
From Guessing to Clinical Certainty Using INSiGHT Scanning to Track Stress-Related Change
This is the moment where modern chiropractic stops living in the world of “I think” and steps into the world of “we know.” Patients with neurological symptoms of stress want answers that feel concrete. What does this mean for me. How do we know it’s changing. What happens if I stop. Without an objective anchor, the conversation turns into over-explaining and hoping the patient buys the story. With objective data, the conversation becomes calm. You are not trying to prove stress exists. You are showing how the nervous system is functioning today and giving a baseline you can revisit.
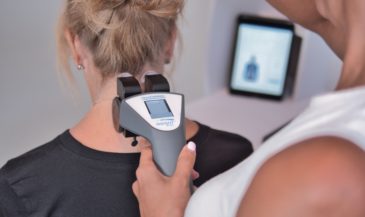
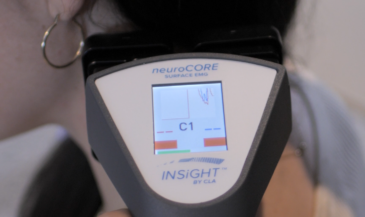
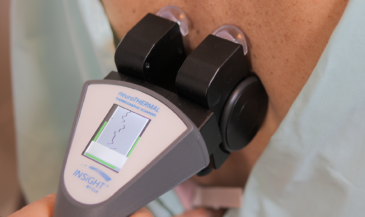
This is where INSiGHT scanning technologies fit naturally. The INSiGHT does not create a care plan. It provides objective exam data and scan reports that support your clinical interpretation. If you want to explore how chronic stress is showing up in function, you need a starting point and a way to track trends. That is exactly what scanning provides. neuroPULSE HRV helps you discuss the stress response through the lens of the autonomic nervous system, including how the patient’s system is adapting, recovering, and responding over time. neuroTHERMAL supports the conversation around stress-related neurological trends by visualizing segmental thermal asymmetries that can be monitored across visits. neuroCORE sEMG connects the stress conversation to muscle activity and motor tone reactions, which matters when stress hormones like cortisol keep the body guarded and reactive. Many patients living in persistent stress show up with chronic tension, headaches, and sensitivity. sEMG lets you discuss changes in electrical activity objectively and track improvements as the patient stabilizes.
Here is the simplest workflow that keeps you in clinical certainty. Establish baseline scans. Tie the findings to symptoms of stress the patient already recognizes, like brain fog, headaches, sleep disruption, dizziness, or tingling. Then re-scan to show trends. That one shift turns stress management from advice into direction. It also makes lifestyle support easier to deliver without being preachy. You can reinforce relaxation, deep breathing, consistent movement that supports an endorphin response, and routines that reduce stress by helping the system downshift. Stress levels do not have to be guessed at. When you can track response patterns, you improve communication, increase follow-through, and make the neurological symptoms of stress easier for patients to understand and easier for chiropractors to manage.
- Establish a baseline and document the patient’s symptoms of stress and functional goals.
- Use objective scans to support your interpretation of nervous system functions and recovery capacity.
- Re-assess and re-scan to show trends when stress persists or when improvement is expected.
- Use the visuals to reinforce ways to manage stress and stress effectively without overwhelm.
The Takeaway That Changes the Conversation
Neurological symptoms of stress are common, real, and often predictable when the stress response becomes chronic. You are not dealing with a patient who is weak or dramatic. You are often seeing a nervous system that has been forced to run in survival mode for too long. Stress affects the nervous system, stress affects the brain, and stress on neurological health shows up as a range of neurological complaints that touch cognition, sleep, pain, sensation, and mood.
As chiropractors, your advantage is consistency and clarity. You can recognize the signs, speak to the impact that stress has on function, and know when a neurologist should be involved for neurological conditions that require medical evaluation. You can also acknowledge the wider reality, including stress-related concerns in mental health disorders, post-traumatic stress disorder, and broader mental health conditions, without pretending you are practicing psychotherapy. You can keep the conversation in your lane and still be incredibly helpful.
And when you anchor the conversation to objective neurological scanning, you remove the guesswork. You move from opinion to evidence, from confusion to clarity, and from vague reassurance to a trackable plan. That is why INSiGHT scanning belongs in this conversation. If the effects of stress are showing up as neurological symptoms of stress, then your best next step is to measure, interpret, and re-check. That is how chiropractors elevate care, increase certainty, and help patients feel progress they can understand.