In chiropractic offices, dysautonomia often appears long before the term is ever used. Dysautonomia patients may describe dizziness, palpitations, orthostatic lightheadedness, fatigue, brain fog, exercise intolerance, or digestive disruption. These dysautonomia symptoms may fluctuate daily, creating an array of symptoms that seem unrelated at first glance. Dysautonomia can affect how patients stand, move, recover, and function, even when they appear outwardly fine.
This matters deeply for chiropractors because dysautonomia is not rare. Estimates suggest that nearly 70 million people worldwide are affected by various forms of dysautonomia. Yet there remains a significant lack of awareness, leaving many people with dysautonomia struggling to find providers who understand autonomic nervous system dysfunction. Chiropractic, when grounded in neurological analysis and objective data, is uniquely positioned to help bring clarity to this complex condition.
Understanding Dysautonomia Through a Neurological Lens
Dysautonomia is an umbrella term used to describe disorders of the autonomic nervous system. In other words, dysautonomia is an umbrella term that encompasses multiple nervous system disorders where involuntary regulation breaks down. Dysautonomia is not a single diagnosis, nor is it a single disorder with one predictable presentation. Instead, dysautonomia can range from mild and intermittent to severe and disabling.
The autonomic nervous system governs processes the body performs without conscious thought. These include heart rate, blood pressure, breathing rhythms, digestion, circulation, pupil response, and sweat production. When autonomic nervous system disorders develop, these functions may fluctuate or fail to adapt appropriately to stress, posture, or activity. Dysautonomia have trouble regulating these processes, which explains why patients often experience different symptoms across multiple systems.
From a chiropractic perspective, it is critical to understand scope. Chiropractors do not diagnose dysautonomia. Diagnosis and treatment decisions, including medical testing such as a tilt table test, fall within medical neurology and cardiology. However, chiropractors can recognize patterns of autonomic dysfunction and autonomic nervous system dysfunction, especially when patients present with orthostatic complaints, blood pressure instability, and nervous system fatigue.
Dysautonomia may also be invisible during short clinical encounters. A patient’s blood pressure and heart rate may appear normal at rest, yet become unstable later in the day. This variability is why dysautonomia depends so heavily on pattern recognition and trend tracking rather than single data points. Understanding dysautonomia through a neurological lens allows chiropractors to focus on nervous system performance rather than chasing isolated symptoms.
Dysautonomia Symptoms and Common Clinical Patterns Chiropractors Observe
One of the defining characteristics of dysautonomia is the sheer breadth of symptoms. Dysautonomia include cardiovascular, neurological, gastrointestinal, thermoregulatory, and energy-related traits. These symptoms of dysautonomia often fluctuate, making diagnosis of dysautonomia challenging for both patients and providers.
Common symptoms include dizziness, lightheadedness, palpitations, fatigue, brain fog, headaches, abnormal sweat responses, temperature intolerance, and difficulty with upright posture. Orthostatic intolerance is a hallmark feature, describing difficulty tolerating standing due to abnormal regulation of blood pressure and heart rate. Orthostatic symptoms may worsen with heat, dehydration, stress, or prolonged standing.
Cardiovascular and Orthostatic Patterns
Cardiovascular dysautonomia symptoms are among the most disruptive. Patients with dysautonomia frequently report unstable blood pressure, rapid or irregular heart rate, and palpitations. Orthostatic hypotension is one presentation, where blood pressure drops when standing. Another common form of dysautonomia is postural orthostatic tachycardia syndrome, sometimes shortened to POTS or pot, where heart rate rises excessively upon standing without a significant drop in blood pressure.
Postural tachycardia syndrome highlights how blood pressure and heart rate regulation is central to autonomic nervous system dysfunction. These orthostatic patterns contribute directly to fatigue, exercise intolerance, and cognitive difficulty. Patients with dysautonomia have trouble standing still, standing in lines, or transitioning from sitting to standing.
Neurological and Systemic Symptoms
Neurological symptoms such as brain fog, light sensitivity, headaches, and difficulty concentrating are frequently associated with dysautonomia. These autonomic symptoms reflect disrupted cerebral blood flow and stress adaptation rather than isolated neurological disease.
Gastrointestinal symptoms are also common. Dysautonomia may include nausea, bloating, constipation, diarrhea, or reflux, reflecting impaired digestion and motility. Thermoregulatory issues such as abnormal sweat patterns, heat intolerance, or frequent chills further point to autonomic nervous system disorders. Many people with dysautonomia experience many symptoms simultaneously, creating debilitating symptoms that impact daily life.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Types and Causes of Dysautonomia Relevant to Chiropractic Care
There are various forms of dysautonomia, and understanding this variability helps chiropractors communicate clearly without oversimplification. Dysautonomia can range from mild to severe depending on the underlying cause and nervous system reserve.
A useful framework distinguishes between primary and secondary dysautonomia. Primary forms occur when dysautonomia itself is the main issue. Secondary dysautonomia develops in association with another condition affecting the nervous system.
Primary Dysautonomia
One form of dysautonomia often referenced is familial dysautonomia, a rare inherited condition affecting autonomic and sensory nerve development. Familial dysautonomia is uncommon but illustrates that some autonomic disorder patterns have genetic origins. Other primary presentations may be idiopathic, meaning no clear cause is identified despite thorough evaluation.
Secondary Dysautonomia and Associated Conditions
Secondary dysautonomia is far more common in chiropractic practice. Dysautonomia may be associated with conditions such as Ehlers-Danlos syndrome, diabetes, autoimmune processes, post-viral syndromes, neuropathy, and autonomic dysfunction or autonomic neuropathy. Neurodegenerative conditions such as multiple system atrophy are also associated with severe autonomic nervous system dysfunction.
Dysautonomia can also be associated with connective tissue instability, chronic stress, and inflammatory processes. Patients often arrive informed by organizations such as Dysautonomia International or resources from the National Institutes of Health, including the National Institute of Neurological Disorders and Stroke information page. This reflects growing public awareness, but also highlights how fragmented care can be.
Diagnosis, Medical Testing, and Where Chiropractic Fits
Diagnosing and treating dysautonomia can be challenging because symptoms may fluctuate and span multiple systems. Many people with dysautonomia experience delays before providers attempt to diagnose dysautonomia in a meaningful way. Diagnosis and treatment often involve collaboration across specialties.
Medical diagnosis may include a tilt table test to assess orthostatic responses, cardiovascular testing to evaluate heart rate and blood pressure, and autonomic testing to assess sweat and reflex responses. These tools help clinicians identify postural orthostatic tachycardia syndrome, orthostatic hypotension, and other autonomic nervous system disorders.
Chiropractors do not diagnose dysautonomia or provide a cure for dysautonomia. However, chiropractors play a valuable role by recognizing autonomic nervous system dysfunction patterns, supporting diagnosis and treatment conversations, and contributing objective neurological analysis. In chiropractic practice, this includes:
- Recognizing orthostatic patterns and frequent symptoms tied to posture or stress
- Encouraging appropriate medical referral when symptoms that need urgent care are present
- Documenting triggers, timelines, and increase in symptoms
- Using objective analysis to track nervous system trends over time
This approach supports appropriate treatment while staying within scope.
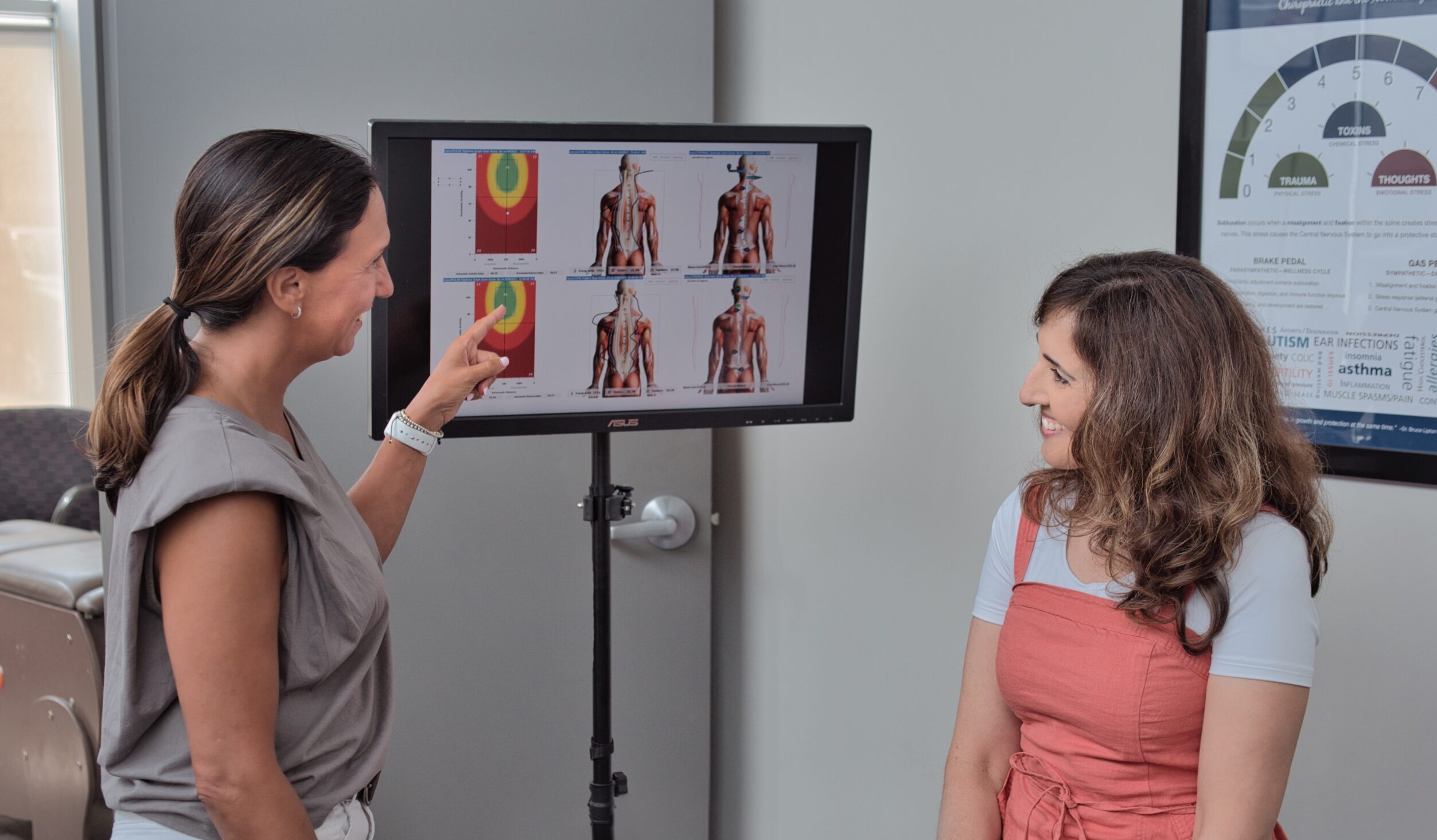
Neurological Scanning and Dysautonomia Conversations in Chiropractic Practice
Dysautonomia patients experience variability. Symptoms may improve one day and worsen the next, even when underlying regulation is slowly changing. This is why neurological scanning is essential in dysautonomia in patients. Objective analysis allows chiropractors to track nervous system performance rather than relying on symptoms alone.
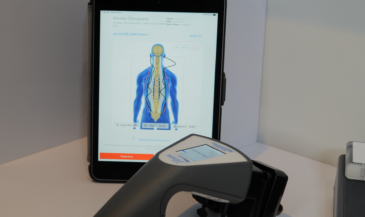
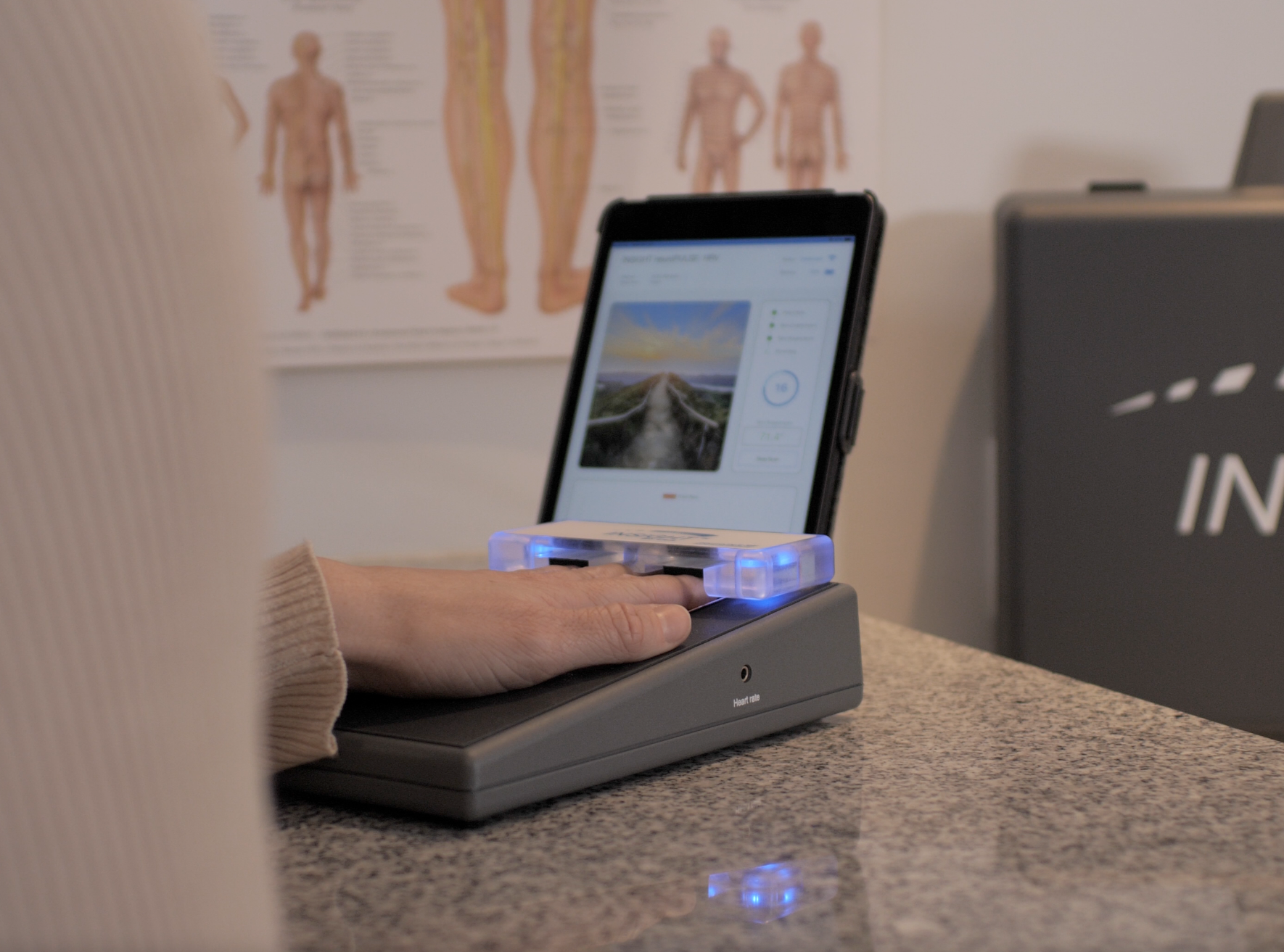
INSiGHT scanning technology provides exam data that supports diagnosing and treating dysautonomia conversations without overstepping scope. neuroPULSE evaluates heart rate variability, offering insight into autonomic nervous system balance, adaptability, and reserve. For patients with dysautonomia who struggle with heart rate and blood pressure regulation, this data helps explain patterns and guide communication.
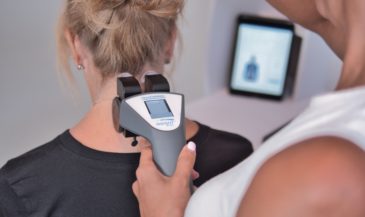
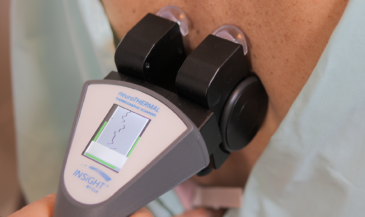
The neuroTHERMAL analyzes segmental autonomic patterning through skin temperature differentials. This is especially relevant for patients experiencing thermoregulatory issues, abnormal sweat responses, and regional stress patterns associated with dysautonomia.
The neuroCORE sEMG evaluates motor tone reactions and energy expenditure, completing the neurological picture. Dysautonomia can also involve postural fatigue and exercise intolerance, making motor system analysis an important part of understanding the full nervous system story.
Together, these tools help chiropractors track trends, support managing dysautonomia conversations, and explain why symptoms are manageable even when they fluctuate.
Making Sense of Dysautonomia Through Nervous System Performance
Living with dysautonomia is challenging because the condition is unpredictable. People with dysautonomia may feel dismissed when tests appear normal, yet their symptoms persist. Dysautonomia patients experience frustration not because symptoms are imaginary, but because regulation is inconsistent.
Chiropractic contributes clarity by focusing on nervous system performance. Rather than promising a cure or oversimplifying complex nervous system disorders, chiropractors use objective analysis to support appropriate treatment and improve symptoms over time. INSiGHT scanning technology helps make the invisible visible, supporting communication, confidence, and collaboration.
Dysautonomia is complex, but chiropractic does not need to be complicated. When care is grounded in neurological insight, pattern recognition, and objective analysis, chiropractors can lead with certainty while supporting patients through one of the most misunderstood autonomic conditions today.
Frequently Asked Questions
What is the disorder called dysautonomia and how does it relate to the autonomic nervous system?
Dysautonomia is an autonomic disorder in which the autonomic nervous system (ANS) does not function properly, causing disruptions in involuntary processes such as heart rate, blood pressure, digestion, temperature regulation, and sweating. Chiropractors should understand that dysautonomia is a broad category of conditions rather than a single disease, and that these dysfunctions can produce specific symptoms in multiple body systems.
How can chiropractors help diagnose autonomic disorder and what are common diagnostic approaches?
Chiropractors do not typically make definitive medical diagnoses of autonomic disorder, but they can identify red flags and refer patients for formal testing. Common diagnostic approaches include tilt-table testing for orthostatic intolerance, heart rate variability, sudomotor testing, and autonomic reflex screens performed by neurologists or cardiologists.
What are the common symptoms of dysautonomia that chiropractors should recognize?
Common symptoms include lightheadedness or fainting on standing, rapid or irregular heart rate, blood pressure fluctuations, chronic fatigue, gastrointestinal disturbances, temperature intolerance, and sweating abnormalities. People with dysautonomia have trouble regulating everyday autonomic functions, so chiropractors should note patterns such as orthostatic intolerance, exercise intolerance, and multisystem complaints that suggest referral for further evaluation.
What type of dysautonomia might a chiropractor encounter in practice?
Chiropractors may encounter several types of dysautonomia, including postural orthostatic tachycardia syndrome (POTS), neurogenic orthostatic hypotension, familial dysautonomia (rare), and small-fiber neuropathy with autonomic involvement. Recognizing the type of dysautonomia helps determine when to suggest specialist referral, and what conservative measures or accommodations might be helpful alongside a formal treatment plan.
How is orthostatic intolerance related to dysautonomia and why is it important for patient care?
Orthostatic intolerance—a core feature of many autonomic disorders—manifests as symptoms like dizziness, palpitations, or fainting when standing up. It is important because it increases fall risk and limits daily activities. Chiropractors should screen for orthostatic intolerance during assessment, advise immediate safety measures, and coordinate with medical providers for diagnostic testing and management strategies.
What treatment options and treatment plan components are used for the treatment of dysautonomia?
Treatment options are usually multidisciplinary and individualized, including hydration and salt-loading, compression garments, graded exercise and physical therapy, medication to stabilize heart rate and blood pressure, and interventions targeting specific symptoms (e.g., GI or pain management). A good treatment program or treatment plan combines medical management, lifestyle modifications, and rehabilitative therapies; chiropractors can contribute to conservative care (manual therapy, exercise guidance) while liaising with the treating physician.
How can chiropractors advise patients on living with dysautonomia and daily self-management?
Chiropractors can educate patients on energy conservation, activity pacing, hydration, salt intake (when appropriate), gradual exercise programs, compression stockings, and strategies to avoid triggers of orthostatic intolerance. They can also help create a practical treatment program that complements medical care and provide resources such as a dysautonomia information page or referrals to dysautonomia project groups for peer support.
What causes dysautonomia and how do the causes influence treatment of autonomic dysfunction?
Causes vary and may include autoimmune processes, genetic conditions, nervous system injury, viral triggers, metabolic diseases, or idiopathic origins. Identifying the cause influences the treatment of autonomic dysfunction—autoimmune cases may require immunotherapy, neuropathic causes focus on nerve regeneration and symptom control, and secondary dysautonomia targets the underlying illness. Accurate cause identification guides specific symptoms management and long-term planning.
When should a chiropractor refer a patient to specialists for further evaluation of dysautonomia?
Refer promptly when patients present with recurrent syncope, severe orthostatic intolerance, rapidly progressive autonomic symptoms, signs of cardiac involvement, or when conservative measures fail. Early referral to cardiology, neurology, or autonomic specialists ensures comprehensive testing (tilt-table, autonomic reflex screens) and formulation of an effective treatment plan. Collaboration with the medical team improves outcomes for people with dysautonomia who have trouble managing complex multisystem symptoms.