That question carries more weight than most realize. Patients are not just asking about a spinal disc. They are asking whether their lower back will ever feel normal again, whether the numbness or tingle in their leg will subside, and whether they can return to normal activities without fear. In the chiropractic industry, we hear this daily. And the answer requires more than a simple yes or no.
So can herniated discs heal? In many cases, yes. A herniated disc can heal without surgery, symptoms often improve, and people regain function. But healing is not instant, and it is not purely structural. The recovery process depends on nerve involvement, inflammation, movement patterns, and overall health. When chiropractors understand that, we guide patients with more clarity and confidence.
What a Herniated Disc Actually Is and Why Symptoms Occur
To answer whether a herniated disc can heal, we first need to understand what a disc herniation really is. Each vertebra in the spine is separated by a spinal disc that acts as a shock absorber. That spinal disc has an outer layer called the annulus and a gel-like center called the nucleus pulposus. When the annulus weakens from wear and tear or overload, the nucleus can push outward. This protrusion of disc material is what we call a herniation.
A herniated disc does not automatically cause severe pain. Symptoms usually arise when there is inflammation or pressure on nearby nerves. The affected area becomes sensitive, and the nerve may transmit pain, numbness, or a tingle sensation. This is why two patients with a similar disc herniation can experience completely different levels of discomfort.
Location matters. A cervical spine herniation may create arm symptoms, numbness in the fingers, or neck stiffness. A lumbar disc herniation in the lower back may lead to leg discomfort, weakness, or classic sciatica when pressure on nerves affects the sciatic nerve pathway. The severity of the herniation does not always predict the severity of symptoms. The nerve response and inflammation often determine how intense the experience feels.
This is where chiropractic thinking becomes important. We are not only evaluating the disc. We are evaluating the spine, the nerve, and how the body adapts. An x-ray may not show the spinal disc clearly, but imaging can reveal alignment and structural stress. More importantly, we assess function. A disc herniation is a structural event. The symptoms are neurological.
Can Herniated Discs Heal? Understanding the Natural Healing Process
Let’s address the central question clearly. Can herniated discs heal? Yes, many can. In almost 90 percent of cases, symptoms improve over time. A herniated disc heal outcome often occurs through natural healing mechanisms, even when no surgery is performed.
There are three primary biological processes that allow a herniated disc to heal:
- Spontaneous retraction, where the portion of the disc that has protruded moves slightly back toward its original position.
- Dehydration and shrinkage, where the gel-like center loses water content and reduces in size.
- Immune reabsorption, where the body recognizes displaced disc material as foreign and breaks it down.
These processes reduce pressure on nerves and allow inflammation to subside. When inflammation decreases, severe pain often diminishes, and symptoms improve. A patient may still technically have a disc herniation visible on imaging, but function returns and nerve irritation calms.
The timeline varies. Some people notice improvement in two to six weeks. Many experience meaningful relief within six to twelve weeks. Complete disc heal remodeling may take six to twelve months. Whether a herniated disc fully normalizes on imaging is less important than whether the patient achieves full recovery in function and comfort.
Can herniated discs heal without surgery? In many cases, yes. Conservative care supports the body’s natural healing mechanisms. The key is managing inflammation, protecting the affected disc, and restoring movement gradually.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Factors That Influence Whether a Herniated Disc Heals
When patients ask whether a herniated disc can heal, they want certainty. The truth is that healing depends on multiple factors. The severity of the herniation plays a role. A mild bulge may resolve quickly, while a larger extrusion of disc material can take longer. However, the severity of the herniation is not the only predictor.
The degree of nerve involvement is critical. Back pain alone often resolves faster than cases with persistent numbness or weakness. If pressure on nearby nerves continues, recovery may extend. A lumbar case with sciatic nerve irritation may require more structured support than a localized cervical discomfort.
Inflammation is another variable. High inflammation keeps the nerve reactive and sensitive. Reducing inflammation is essential for the disc to heal effectively. Patient overall health also matters. Blood flow, sleep, nutrition, and smoking habits influence tissue recovery. Poor lifestyle habits can worsen healing time and delay the recovery process.
Posture and ergonomics influence mechanical stress. If the patient continues poor lifting patterns or prolonged flexion, the disc may not settle. Adherence to the care plan is essential. Physical therapy exercises and therapy exercises that strengthen core muscles and improve flexibility protect the spine. Consistency prevents setbacks.
If symptoms worsen, especially with bladder or bowel changes, immediate evaluation is required. Patients should see a doctor when progressive numbness or weakness appears. These are red flags and require diagnostic tools beyond conservative monitoring.
Conservative Care That Supports Herniated Disc Recovery
Most chiropractors begin with non-surgical strategies because many herniated discs heal without surgery. Conservative treatment options aim to reduce inflammation, restore motion, and prevent recurrence.
Early management often includes:
- Short-term rest without complete immobilization.
- Cold therapy to reduce inflammation.
- Activity modification to protect the affected area.
As the acute phase settles, movement becomes essential. Physical therapy and physical therapy exercises focus on lumbar stabilization, core muscle activation, and improving range of motion. Low-impact aerobic activities enhance blood flow and promote healing. A physical therapist can guide progression safely.
Anti-inflammatory medications may reduce inflammation short term, but should not be used long-term without supervision. Lifestyle adjustments support the recovery process. Weight management, quitting smoking, and ergonomic improvements help prevent future episodes.
In persistent cases, minimally invasive procedures such as microdiscectomy may be recommended. During surgery, the disc is removed from the irritated nerve region. However, even when surgery is performed, rehabilitation and structured progression remain essential to prevent future disc herniation.
Why Objective Neurological Scanning Changes the Conversation
In chiropractic practice, the question can herniated discs heal is not only structural. It is neurological. Symptoms fluctuate. A patient may report reduced pain one week and renewed tingle the next. That does not always mean the disc is worsening. It often reflects nervous system sensitivity.
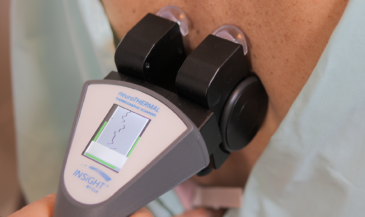
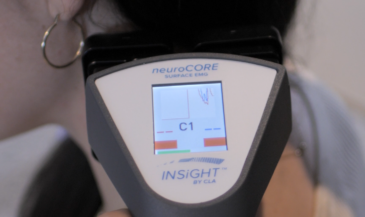
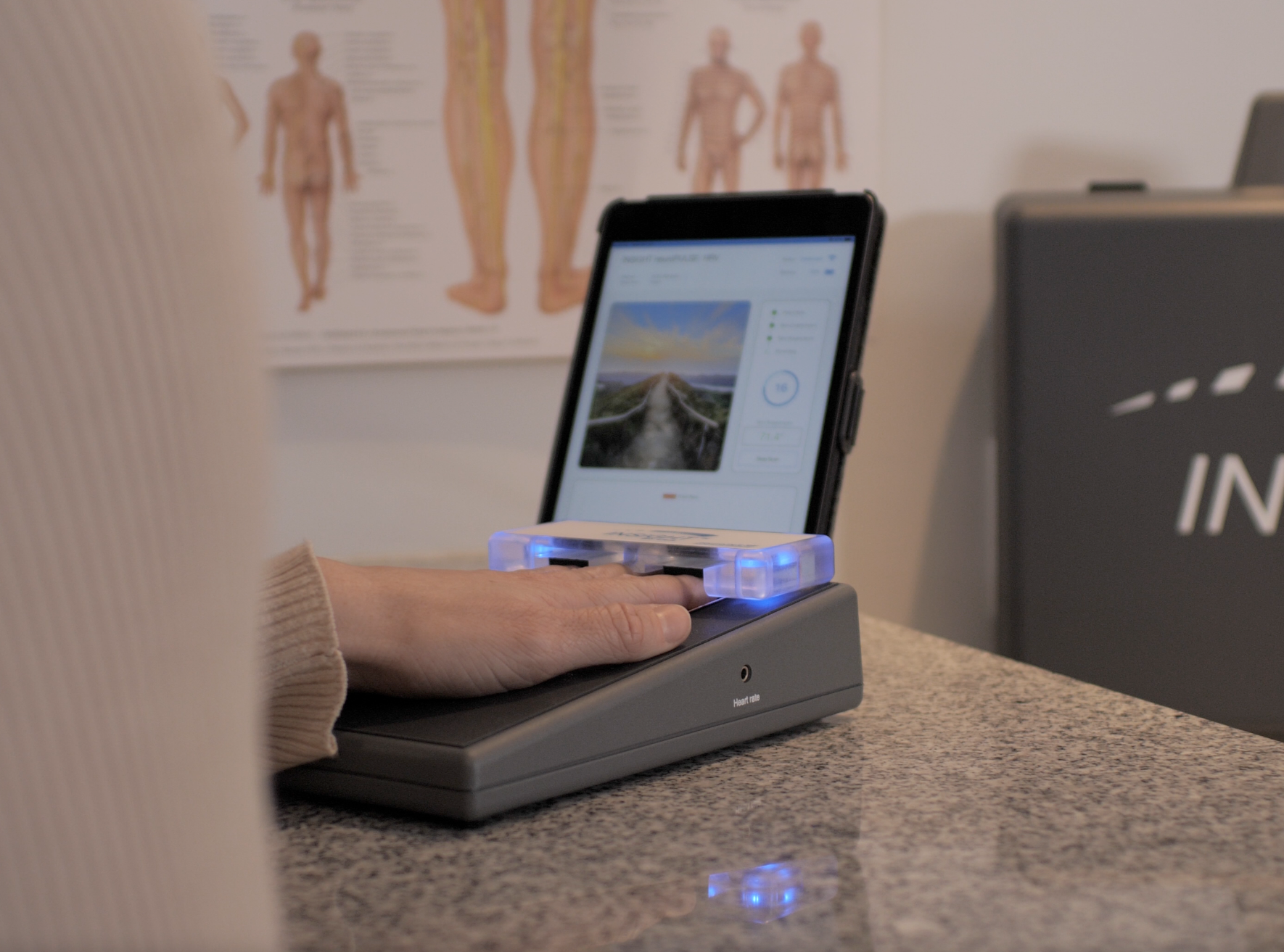
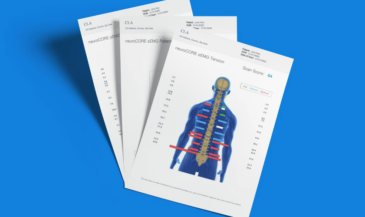
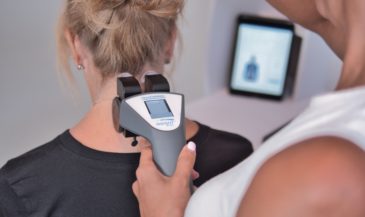
This is where INSiGHT scanning technology becomes clinically valuable. The INSiGHT neuroTECH and Synapse software provide objective exam data that help chiropractors evaluate nerve tension, postural tension, and autonomic patterns around the spine. While imaging evaluates structure, scanning evaluates function.
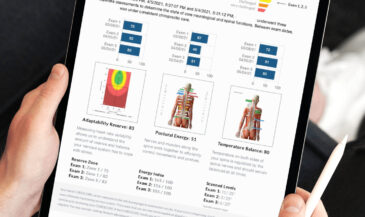
The neuroTHERMAL scan assesses segmental stress patterns that may correlate with irritation and inflammation. The neuroCORE sEMG evaluates muscular compensation and how the spine stabilizes around the affected disc. The neuroPULSE HRV analysis evaluates adaptability and resilience, which influence how the body handles neurological distress.
When a patient asks can herniated discs heal, you can now answer with data. You establish a baseline and track trends over time. Even if imaging remains unchanged, functional improvements can demonstrate that the herniated disc is healing in a meaningful way. Objective trends turn uncertainty into direction.
Scanning also strengthens adherence. Patients often stop care once pain decreases. But a disc herniation recovery plan is about restoring nervous system performance, not just reduced pain. Objective analysis helps explain why continued care supports stability and helps prevent future flare-ups.
Bringing It All Together for Disc Healing and Long-Term Stability
So can herniated discs heal? Yes, many can. A herniated disc heal outcome often occurs through natural biological processes, conservative care, and time. Most patients experience symptom relief within weeks to months, and many return to normal life without surgery.
But healing is not just about the spinal disc. It is about the nerve, inflammation control, structured rehabilitation, and overall health. It is about protecting the affected disc while building resilience in the spine. It is about restoring posture, improving flexibility, strengthening core muscles, and ensuring the nervous system can adapt.
As chiropractors, our responsibility is not to promise perfect imaging. It is to guide a clear recovery process. When patients understand how the disc may heal, why symptoms improve, and how objective neurological scanning tracks progress, fear decreases. Confidence grows. And long-term outcomes improve.
When the next patient asks can herniated discs heal, you can answer confidently. Yes, many do. And with the right care plan, conservative support, and objective tracking using INSiGHT scanning technology, you can guide them toward stability, resilience, and full recovery.