Sympathetic overdrive is one of the most common reasons a patient feels like they are stuck in a state of stress, even when nothing is actively threatening them. Their system is trying to protect them, but it is doing it too often and for too long. When that happens, the conversation can get messy fast unless you have a clean way to explain what is happening and a clear way to track change.
That is where modern chiropractic communication wins. When the conversation is only about symptoms, it becomes emotional and inconsistent. When the conversation is scan-led, it becomes measurable, calm, and practical. You are not trying to convince anyone. You are simply showing what the nervous system is doing today and what it does next.
Why Sympathetic Overdrive Shows Up in Chiropractic Conversations
Sympathetic overdrive walks into your office wearing a lot of different outfits. One patient comes in for headaches. Another comes in for “tight shoulders.” Another says they are exhausted but cannot sleep. Another is dealing with chronic pain and feels like their body is always bracing. When you zoom out, the common thread is regulation. The system gets reactive, stays reactive, and then struggles to recover.
In simple terms, sympathetic overdrive is persistent, excessive activation of the body’s stress response. It is sometimes described as sympathetic overactivity, and it can feel like being stuck in “fight or flight” even without immediate danger. In the report of findings, I often describe it as the accelerator being pressed too easily and the brakes not engaging smoothly. That is the lived reality of a nervous system cannot calm.
Clinically, this matters because the patient is not just dealing with a local complaint. They are often dealing with nervous system performance that is out of rhythm. If you only chase the complaint, you miss the bigger story. If you recognize sympathetic overdrive early, you can explain it clearly, set expectations realistically, and build a care plan that is grounded in objective findings and re-checks.
- Patients often describe being tired but wired, especially at night
- They may feel irritable and short-tempered in ways that do not feel like them
- They may report brain fog and reduced focus
- They may mention digestive problems or a nervous stomach during busy days
- They often struggle with staying asleep or waking unrefreshed
Here is the key chiropractic takeaway. Sympathetic overdrive is rarely solved by better advice alone. It is solved by better clarity. When you can define what is happening, track it, and show progress, patients stop guessing and start following a plan with more confidence.
The Autonomic Nervous System Explained for Chiropractic Application
To keep this topic useful in practice, we have to keep it simple and accurate. The body has an automatic regulator called the autonomic nervous system. You will also hear it shortened to ANS or ans. This is the network that helps regulate functions you do not consciously control, like heart rate, breathing rhythm, digestion, and vascular tone. In other words, it is the automatic system that decides whether the body should speed up or slow down.
The autonomic nervous system has two main branches that counterbalance each other. The sympathetic nervous system, often shortened to SNS or sns, is the accelerator. It drives the sympathetic response that prepares the body to act. It is the body’s “fight or flight” mechanism and it is essential. The parasympathetic nervous system is the braking system. It is your “rest and digest” branch, supporting calm, digestion, recovery, and restorative processes. A resilient person is not someone who never uses the accelerator. A resilient person is someone who can accelerate and then settle.
When someone is in sympathetic dominance, the issue is not that the sympathetic nervous system turns on. The issue is that it stays elevated too long, too easily, or too often, especially during prolonged stress. Over time, that can be paired with stress hormones like cortisol. Cortisol is not automatically bad, but cortisol levels that stay elevated can reinforce a dysregulated stress response. The physiology often looks predictable: increased heart rate, vascular changes that can contribute to high blood pressure, and reduced digestive resources because blood flow gets redirected away from the gut in a fight-or-flight state.
This is also where chiropractors can speak with both confidence and restraint. The vagus nerve is a major parasympathetic pathway involved in calming and digestion. When the vagus nerve is not engaging well, patients may describe difficulty settling, poor digestion, and light sleep. In chiropractic conversations, the cervical spine is sometimes part of the broader discussion of regulation because it is a region where patients commonly carry protective tension and where chiropractors evaluate function. The goal is not to make simplistic claims. The goal is to explain regulation, evaluate what you can evaluate, and track whether the person is trending toward a more balanced state.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
How Sympathetic Overdrive Presents and What It’s Commonly Associated With
If you want to spot sympathetic overdrive quickly, listen for the theme of reactivity. The patient reacts bigger than the moment calls for, and they stay activated longer than they should. They may report an elevated heart rate after small stressors, or they may describe that their heart rate feels high even when they are trying to rest. In some cases, you will also see a history of hypertension, high blood pressure, or new concerns about high blood pressure trends. That does not mean every patient is hypertensive, but sympathetic nervous system activity is closely tied to how the cardiovascular system responds under load.
Here is what this presentation often looks like when you translate it into real-world traits. The list matters because it helps you name what the patient is already experiencing, without overdiagnosing or sensationalizing. When you name it accurately, the patient feels understood and the conversation becomes easier.
- Sleep disruption, including staying asleep issues and a sense that sleep is not restorative
- Brain fog, scattered focus, or mental fatigue that does not match effort
- Anxiety, physical tension, and a sense of being “on edge”
- Digestive problems, reduced appetite, or a nervous stomach during high-demand days
- Muscle guarding and postural bracing, often described as constant tightness
Now let’s talk drivers and associations, because this is where chiropractic communication needs to be careful and useful. Chronic stress is the most common background factor, but it is not just emotional stress. Lifestyle load matters, including irregular sleep timing, constant stimulation, stimulants, and under-recovery. Metabolic strain can also be part of the story, including associations with type 2 diabetes. Sleep-disordered breathing is another big one. Obstructive sleep apnea can keep the system in repeated night-time fight-or-flight loops, which can maintain a dysregulated stress response even if the patient thinks they are “sleeping.” You may also hear broader labels tied to autonomic regulation challenges, including dysautonomia. Chiropractors should not diagnose complex medical conditions from a conversation, but you can recognize when the pattern sounds like an overactive sympathetic nervous system and respond by gathering objective findings and communicating clearly.
One more practical point for your report of findings. Patients often think the answer is simply “less stress.” The more helpful frame is regulation. The root of the problem is often that the system is trained to react faster and recover slower. If you can show that clearly and track it, the patient stops seeing this as personal weakness and starts seeing it as physiology that can improve.
Making It Measurable with INSiGHT Scanning Technology
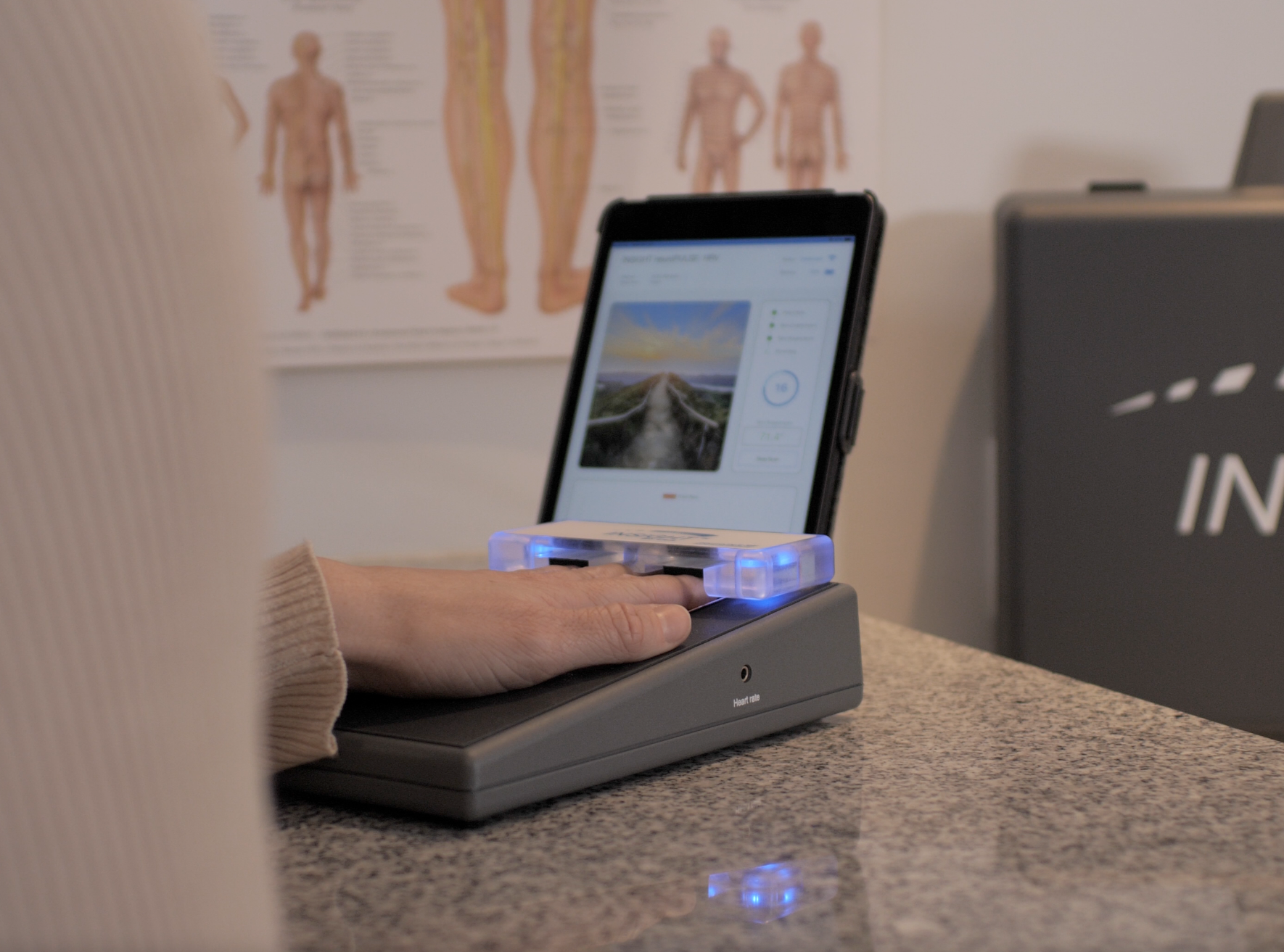
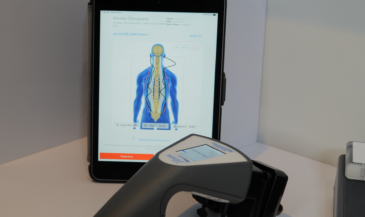
This is the turning point in the conversation. You can explain sympathetic overdrive beautifully, but if the patient cannot see it, they will treat it like a mindset issue. That is where neurological scanning changes everything. INSiGHT scanning technology takes an invisible story and makes it visible. It gives you objective exam data and scan reports so the conversation is grounded in what is happening, not just what is felt.
In sympathetic overdrive cases, chiropractors are trying to quantify adaptability and recovery. Can the system settle after demand, or is it locked in an overactive sympathetic loop? This is one reason heart rate variability can be helpful as part of a broader picture, because it supports a discussion about autonomic regulation and autonomic balance. You are not just looking for a good day. You are looking for a trend that shows the person can shift states and stabilize.
Here is how chiropractors typically use the INSiGHT neuroTECH and Synapse software ecosystem to support clearer communication and cleaner re-checks:
- neuroPULSE supports discussion of autonomic regulation by helping you communicate how the autonomic nervous system is adapting and recovering. It gives you a measurable way to talk about regulation rather than relying only on subjective stress talk.
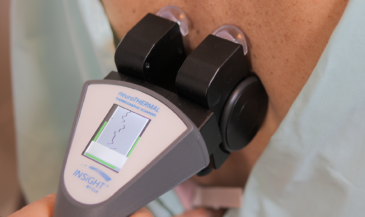
- neuroTHERMAL provides analysis of segmental stress trends that can support a scan-led report of findings and a clearer conversation about neurological distress and stability over time.
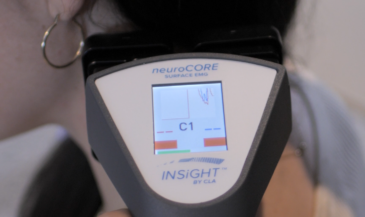
- neuroCORE sEMG evaluates muscle activity and motor tone reactions that often travel with sympathetic system bracing and guarding patterns.
One accuracy point that protects trust. The INSiGHT does not create a care plan. It provides objective analysis and reports. The chiropractor interprets the information, integrates it with the full examination, and then designs the care plan and the re-check schedule. That distinction keeps your communication clean and your patient confident. When you re-scan and the patient can see a shift out of sympathetic overdrive, the conversation becomes less emotional and more practical. They understand why you are doing what you are doing, and they can see when the system is starting to restore balance, rebalance, and move back into balance.
Practical, Drug-Free Strategies Chiropractors Can Recommend to Support a Shift Toward Balance
Once the patient understands sympathetic overdrive, they usually want to know what they can do between visits. The most helpful recommendations are simple, repeatable, and focused on state shifting. The goal is not perfection. The goal is helping the nervous system practice downshifting so the parasympathetic system has room to do its job again. That is how you support better sleep and more consistent regulation.
Here are practical, drug-free strategies that fit naturally into a chiropractic conversation and support the idea of addressing the root without overpromising:
- Diaphragmatic breathing for 2 to 5 minutes once or twice daily. Slower breathing with longer exhalations supports downshifting and can be framed as vagus nerve support for parasympathetic engagement.
- Sleep anchors that protect sleep architecture. Encourage a consistent wake time, reduced evening stimulation, and a short wind-down routine that signals safety. This is especially helpful for patients who struggle with staying asleep.
- Moderate movement, not punishment. A daily walk or gentle mobility can support regulation when the system is already reactive.
- Nutrition and hydration basics. Regular meals with protein and steady hydration reduce volatility in the stress response and can help stabilize energy without relying on stimulants.
- Stimulant step-down when appropriate. If caffeine is masking fatigue while the system is already overactive, reducing it gradually can support steadier regulation.
It is also wise to keep an eye open for contributors that require coordination. If a patient snores loudly, wakes unrefreshed, or reports consistent morning headaches, obstructive sleep apnea should be on your radar for referral conversations. If high blood pressure is consistently elevated, or the patient is already among hypertensive patients, your role is to communicate responsibly and coordinate appropriately. Sympathetic overdrive is associated with sympathetic influence on the cardiovascular system, but chiropractors remain clear about scope while still addressing regulation, recovery, and resilience through measurable care.
From Reactivity to Resilience
Sympathetic overdrive is not rare and it is not mysterious. It is physiology that has been trained by chronic stress, prolonged stress, and modern lifestyle load to stay activated. In that place, the body can feel like it is stuck in “fight or flight” even when nothing is immediately dangerous. Over time, this can show up as brain fog, irritability, sleep disruption, digestive problems, and signs like increased heart rate or high blood pressure trends. It can also overlap with broader regulation challenges such as dysautonomia, and it may be associated with sympathetic patterns seen in hypertension and metabolic strain, including type 2 diabetes. The point is not to label the patient. The point is to recognize the theme and guide the next step.
The chiropractic opportunity is to make this measurable and manageable. When you can explain what is called the autonomic nervous system, show how the sympathetic nervous system and parasympathetic nervous system influence regulation, and track change over time, the conversation becomes simpler. You are no longer asking the patient to guess. You are helping them see what is happening and why. That is how you address the root, not just the complaint. It is also how you build trust during the weeks when life is chaotic and the patient feels like they are sliding backward.
Most importantly, scan-led care keeps the focus on objective progress. When sympathetic overdrive is known as sympathetic overdrive in your office, it becomes a trend you can track and a capacity you can build. INSiGHT scanning technology helps you establish baseline nerve activity, guide clearer communication, and re-check the trend with tools like neuroPULSE, neuroTHERMAL, and neuroCORE sEMG. That is how you help a patient restore balance and move toward a balanced state that supports long-term health, not just short-term relief.