What makes paraspinal tenderness so important is that it rarely exists in isolation. It is frequently associated with low back pain and spine complaints, but it also shows up in patients who downplay symptoms or believe their issue is purely mechanical. In reality, paraspinal tenderness reflects how the nervous system is managing load, stability, and movement around the spine. It can signal acute protection, chronic compensation, or deeper patterns tied to disc behavior, posture, and neurological distress.
For chiropractors, this finding is an opportunity. When you understand the nature of paraspinal tenderness and interpret it through a neurological lens, it becomes more than a sore spot. It becomes a meaningful indicator of spine and paraspinal muscle health, one that can guide examination, communication, and long-term care planning.
Understanding Paraspinal Tenderness in Chiropractic Practice
Paraspinal tenderness refers to soreness, sensitivity, or pain or discomfort felt in the muscles around the spine, typically along the paraspinal musculature adjacent to the vertebra. It may feel localized or widespread, mild or intense, and it often presents alongside pain and stiffness or reduced range of motion. In many cases, it is associated with low back pain due to prolonged sitting, lifting, or repetitive movement, particularly within the lumbar spine and lumbar region.
In chiropractic, it is essential to view paraspinal tenderness as a sign rather than a diagnosis. The tenderness you feel may reflect muscle spasm, protective guarding, or altered muscle function driven by the nervous system. Sometimes it is the result of a clear muscle strain. Other times, it reflects an acute and chronic pattern where the original tissue irritation has resolved, but the body continues to stabilize the spine inefficiently. This is why paraspinal tenderness often fluctuates even when imaging or structural findings appear unchanged.
Clinically, paraspinal tenderness can appear with or without significant symptoms. Some patients with acute pain react strongly to palpation, while patients with chronic pain may show less sensitivity despite long-standing dysfunction. This disconnect highlights why symptoms alone are not a reliable guide. The nervous system may continue to regulate muscles around the spine based on perceived instability, stress on the muscles, or past injury, even when pain has faded.
For chiropractors, paraspinal tenderness becomes a gateway finding. It opens the conversation about how the spinal column is adapting and whether the paraspinal muscles are being asked to do more than they should to stabilize the spine.
Anatomy and Function of the Paraspinal Muscles
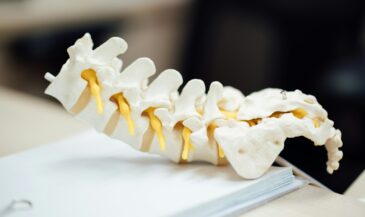
The paraspinal muscles are an extensive network of muscle groups that run along the back of the spinal column, supporting posture, movement, and stability. Understanding the anatomy of the paraspinal system is essential for interpreting paraspinal tenderness accurately. These muscles attach to the lumbar vertebrae, thoracic segments, ribs, sacrum, and pelvis, creating a dynamic support system around the spine.
Superficially, the erector spinae muscles are responsible for extension and gross stabilization. Deeper layers include the multifidus muscle, rotatores, and other paravertebral muscles that fine-tune segmental control. The lumbar multifidus plays a particularly important role in stabilizing individual motion segments in the lumbar spine. When these deep stabilizers are not functioning efficiently, the body often compensates by over-recruiting larger muscles, leading to paraspinal muscle spasm and tenderness.
The relationship between paraspinal muscle function and spinal mechanics is tightly linked to disc behavior. Intervertebral discs and the lumbar intervertebral disc structures help absorb load and allow smooth motion. When disc tolerance changes, whether through degeneration or irritation, the nervous system often increases muscle tone to protect the area. Over time, this can affect muscle structure and function, leading to altered muscle recruitment, reduced muscle strength where it matters most, and even muscle atrophy in chronic cases.
Research consistently shows that patients with acute and chronic low back pain can develop changes in specific paraspinal muscles, including paraspinal muscle atrophy and fatty infiltration, particularly on the symptomatic side. This shift in muscle mass and muscle fibers alters how the spine is stabilized and contributes to persistent tenderness. In these situations, stretching alone is rarely an effective treatment. The issue is not flexibility, but coordination and efficiency.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Causes and Patterns of Paraspinal Tenderness
The causes of paraspinal muscle pain are varied, but they follow recognizable patterns. Mechanical causes remain the most common. A muscle strain, including muscle strain from lifting or twisting, can create acute tenderness and protective spasm. Poor posture, prolonged sitting, and repetitive movements place continuous stress on the muscles, especially during lumbar spine flexion, leading to fatigue and guarding in the lumbar paraspinal tissues.
Trauma is another contributor. Accidents, falls, sports injuries, and even minor impacts can trigger protective responses in the spinal muscle system. In some cases, post-surgical immobility or prolonged inactivity contributes to muscle mass loss and reduced muscle function, increasing vulnerability when normal activity resumes. These patients may present with pain in the lower back, stiffness, and tenderness without a clear new injury.
Degenerative patterns also play a role. Disc changes, back pain and spine degenerative patterns, and pain and spine degenerative disorders can alter load tolerance in the lumbar back. In response, the nervous system recruits muscle to stabilize the spine. This is why paraspinal tenderness is often associated with low back pain and spine issues even when activity levels remain low. A lumbar disc herniation or irritation can provoke guarding that persists well beyond the acute phase.
Neurological distress adds another layer. Chronic sympathetic overdrive can lead to sustained muscle tension, trigger points, and altered muscle tone. Over time, this contributes to chronic paraspinal muscle pain and the familiar cycle of pain where movement feels unsafe, activity decreases, and compensation increases. In these cases, paraspinal muscle pain refers to discomfort that is not purely local, but part of a broader adaptive pattern.
Clinical Interpretation of Paraspinal Tenderness
Paraspinal muscle pain is crucial information during examination, but interpretation matters. Tenderness may reflect a true paraspinal muscle spasm, a protective response to disc irritation, or altered muscle recruitment across the spinal region. Observing how tenderness responds to movement, posture, and palpation helps differentiate acute pain from chronic patterns.
Patients with acute presentations often describe sharp pain, limited range of motion, and clear aggravating factors. Patients with chronic back pain or chronic low back pain may describe diffuse aching, pain associated with prolonged sitting, or pain that fluctuates without clear triggers. In these cases, altered muscle firing and muscle dysfunction often underlie the tenderness you feel.
Palpation alone cannot determine whether the system is overactive, underactive, or inefficient. This is where objective analysis becomes essential. Understanding paraspinal muscle pathophysiology requires more than hands-on assessment. It requires measuring how the spinal muscle system is behaving over time and how it responds to care.
Paraspinal Tenderness Through the Lens of Neurological Scanning
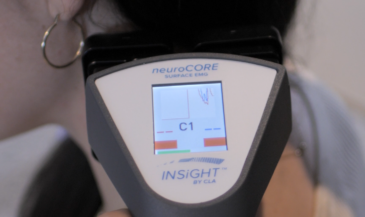
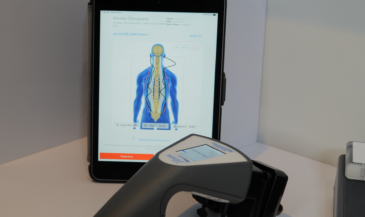
Neurological scanning allows chiropractors to move beyond assumptions and into clarity. INSiGHT scanning technology supports the interpretation of paraspinal tenderness by providing objective insight into motor and autonomic patterns. The neuroCORE sEMG evaluates paraspinal muscle activity, symmetry, and energy expenditure across the spinal column, helping identify inefficient stabilization strategies.
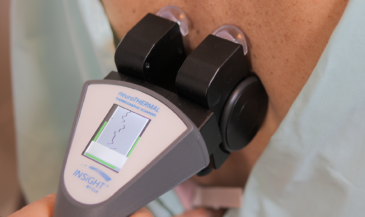
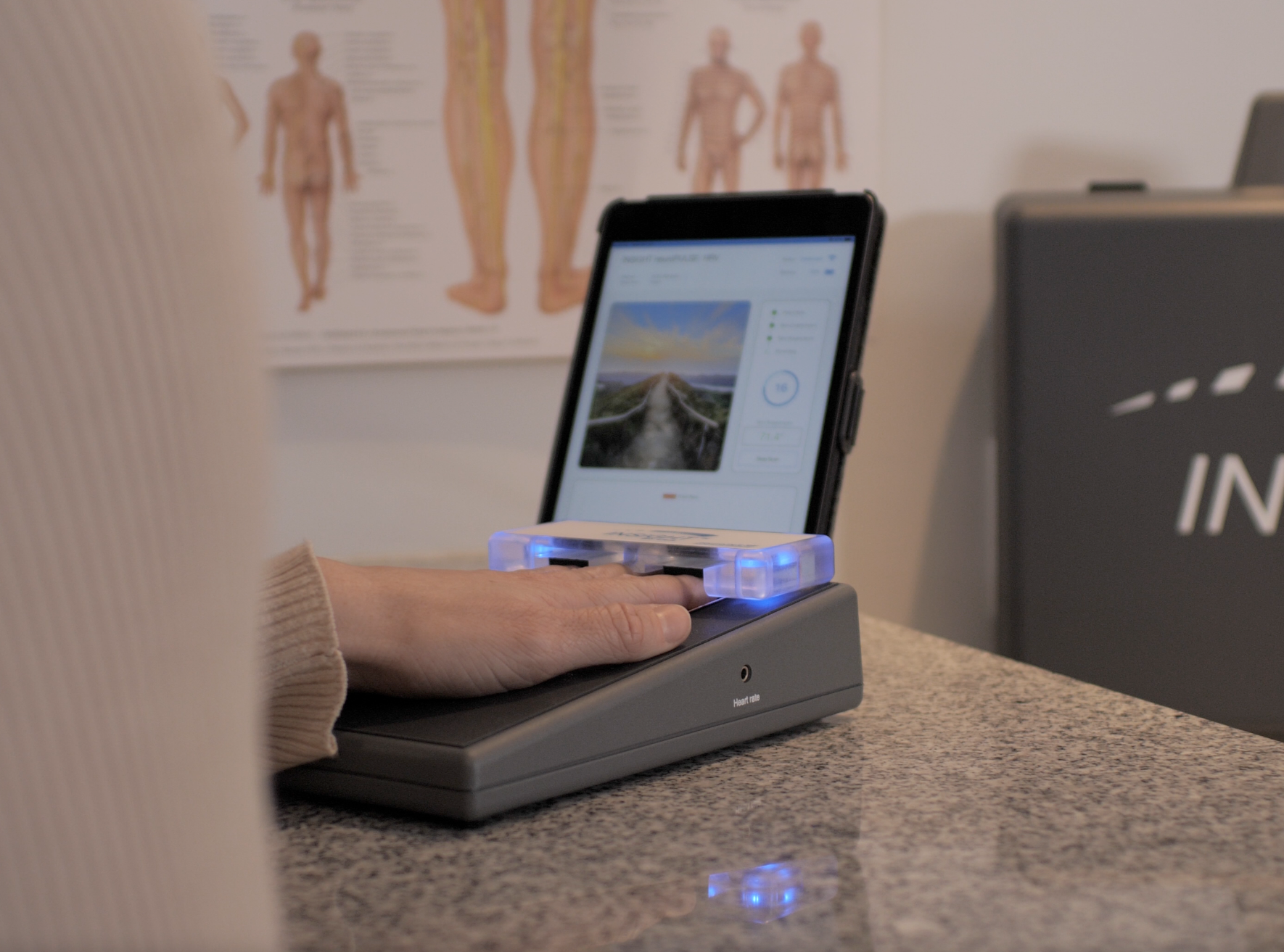
The neuroTHERMAL scan adds autonomic context by assessing temperature patterns around the spine, revealing areas where neurological distress may be influencing muscle behavior. The neuroPULSE HRV scan evaluates adaptability and reserve, offering perspective on how well the nervous system is responding overall. Together, these scans help chiropractors distinguish between acute and chronic paraspinal muscle patterns and track response to treatment.
When scan views are used during reports of findings, paraspinal tenderness becomes understandable to patients. Instead of focusing solely on pain or discomfort, the conversation shifts to how the nervous system is regulating muscles around the spine. This supports clearer treatment plans, more confident treatment options discussions, and proof your care is making a difference through measurable change.
From Tenderness to Understanding in Chiropractic Care
Paraspinal tenderness is not simply a sore muscle. It is a reflection of how the spine, muscles, and nervous system are interacting. When chiropractors recognize its significance, they gain insight into stability, adaptation, and long-term function.
By combining skilled palpation with objective neurological scanning, chiropractors can interpret paraspinal tenderness with greater certainty. This approach supports effective treatment and prevention strategies, improves communication, and reinforces chiropractic’s role in supporting resilient nervous system performance. When tenderness is understood, managed, and tracked appropriately, it becomes a powerful guide rather than a lingering question mark.