In practice, this is where stress can feel confusing. People can feel overwhelmed on a day when their physiology recovers quickly. They can also feel “fine” while their system is running hot under the hood. Stress is both mental and physical, and it doesn’t always announce itself honestly. That is exactly why chiropractors need a better way to talk about stress without turning the report into a motivational speech.
Here’s the shift that makes the whole topic useful. Instead of trying to guess whether your patient is under a normal stress level, help them know your baseline. Then show them what their body is doing when life applies pressure. Whether your stress is low stress, medium stress, or high stress matters less than one question: can the system settle and recover, or does it stay stuck in overdrive?
Normal Stress Level Is Not a Feeling, It’s a Nervous System Baseline
In the chiropractic profession, stress is a daily topic. Patients use it to describe everything from a stressful situation at work to a season of caregiving to a sense that they can’t settle down. They may say they feel stressed. They may say they feel overwhelmed. They may describe tension, irritability, fatigue, or brain fog. Those traits matter, but they are not the same as an objective view of what the autonomic nervous system is doing.
A normal stress level, clinically, is a baseline that can handle everyday stressors and still recover. Everyone experiences stress, and not all of it is harmful. There is good stress, and there is healthy stress. Training, learning, adapting, presenting, traveling, and even positive life change can create demand and still be productive. This is where stress can be positive. It can help you focus, mobilize energy, and respond to a challenge. The issue is not that daily stress exists. The issue is what happens after the pressure passes.
That is why the word “normal” needs a little maturity. A normal range is not one universal number. It depends on genetics, life experiences, sleep patterns, lifestyle changes, fitness, recovery habits, and what the person is carrying right now. Causes of stress include workload, finances, relationships, illness, training load, travel, and time pressure. Two patients can have the same day, face the same stressor, and have completely different physiological responses. One adapts and settles. The other stays elevated. Over time, that is how stress becomes chronic stress.
For chiropractors, the practical takeaway is communication. If you build your conversation on feelings alone, you end up debating. A patient may insist they are fine, or that it is just stress from time to time. The chiropractor may see that their physical health is paying the price, but without an objective anchor, it turns into opinions. This is where scanning matters, because it changes the discussion from “how you feel” to “what your system is doing” and whether your stress is trending toward recovery.
- A normal stress level is not the absence of stress. It is the presence of recovery.
- Good stress and bad stress are separated by one thing: the ability to cope and settle back toward a resting state.
- Stress symptoms can be misleading. They can fluctuate, improve early, or be masked by adrenaline.
- The chiropractor’s advantage is helping the patient understand baseline and trend, not chasing a perfect day.
What the Body’s Stress Response Actually Does
Most patients think stress is a feeling. Chiropractors know it’s a strategy. The body’s stress response exists to protect you. When the brain perceives threat, it initiates activation of the stress response through nerve and hormonal signals. The sympathetic nervous system increases readiness, and the adrenal system releases stress hormones to support immediate survival. That is where adrenaline and cortisol come in. One mobilizes energy quickly. The other supports sustained fuel and changes what the body prioritizes for the moment. In a short window, it is brilliant. It helps your body respond.
In that moment, fight or flight is not a character flaw. It is a survival feature. It sharpens focus, changes circulation, and increases output. You can see it in heart rate and blood pressure, and you can feel it as alertness, tension, or a racing mind. This is also why stress can also show up in places patients don’t expect, like digestion, sleep patterns, and recovery. The effects of stress are not just emotional. They are biological.
The problem is what happens after the stressful event passes. A healthy system should downshift. Your heart rate should settle. Your physiology should move back toward repair and restoration. That ability to return to normal is the difference between a normal stress level and a system that is staying activated too long. When the stressors are constant and there is no real recovery, stress becomes a problem. Over time, that long exposure can affect your health and raise a higher risk for issues patients recognize, including burnout, sleep disruption, and even high blood pressure in the right context. Chiropractors are not diagnosing a mental health condition, but we can absolutely help patients understand when their physiology is stuck and why that matters for mental and physical health.
This is also where good coaching helps. We can encourage patients to take steps to manage the load they can control. We can explain that stress management is not about becoming calm all the time. It is about restoring flexibility, so the system can respond appropriately and then recover. That is an important distinction for patients who believe their only two options are “ignore it” or “break down.”
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Normal in the Real World, Using Wearables and Weekly Averages Without Overpromising
Patients are arriving with data. A watch, a ring, an app. They will tell you their stress level like it is a lab value, and sometimes they will trust the number more than their own body. Other times they will dismiss it completely. Either way, this is an opportunity, because wearables have normalized the idea that nervous system signals can be tracked. The key is to use that curiosity without overpromising what any one metric can do.
Most wearable stress scores are displayed on a 0–100 scale. A practical normal range reference many patients recognize looks like this: 0–25 is a resting state, 26–50 is low stress, 51–75 is medium stress, and 76–100 is high stress. That framework can help patients make sense of their day. But clinically, one spike does not define them. A stressful situation, a hard workout, travel, illness, alcohol, or a bad night of sleep can all raise the level of stress temporarily. That is why a single day is less useful than average stress across a week. The bigger question is whether your stress settles back down, or whether the baseline keeps drifting upward.
This is where you can coach with maturity. Whether your stress is higher on a busy day is not the issue. The issue is whether the patient has enough recovery time built into their week. If their numbers show frequent elevation with little recovery, stress may be shifting from normal demand to chronic stress load. If their wearable shows regular recovery windows, then the system may be adapting well, even if life is busy. Either way, the wearable becomes a conversation starter, not a verdict. It helps you identify triggers your stress responds to and gives you a place to begin a plan that is based on trend, not fear.
When patients ask what to do, keep it practical. There are ways to manage that do not require perfection: consistent sleep timing, smarter training load, hydration, movement, and simple downshifting habits. Deep breathing is a classic because it is immediate and repeatable. So is journaling, light movement, and a wind-down routine. Techniques can help, but they work best when the patient can see how their nervous system responds over time.
HRV and Neurological Scanning, How Chiropractors Objectify Stress and Recovery Capacity
This is where the conversation becomes clearer, because heart rate variability gives you a direct window into adaptability. Heart rate variability is the variation in time between heartbeats, and it reflects how flexibly the autonomic nervous system is shifting between readiness and recovery. When the system is adaptable, those intervals change smoothly. When the system is under load, those intervals tend to become more rigid. Patients don’t need to memorize physiology to understand that. They just need to understand that a normal stress level is closely tied to recovery capacity.
Here’s the clinical maturity piece: HRV is personal. It is not a competition. Your baseline is as individual as a fingerprint, which is why I prefer to talk about trend instead of chasing a perfect number. Acute stress can lower HRV temporarily, and that can be completely appropriate. The question is whether the system rebounds. Chronic stress can suppress HRV over time, and that can be a clue that the body and mind are not getting enough restoration. Patients often feel this as stress and anxiety, irritability, fatigue, and poor recovery. It is mental and physical, and the line between them is not always clean. That is why objective measurement is so useful, because it helps you coach without judging and communicate without guessing.
In the report of findings, this gives you a simple framework. First, help the patient developing a mental understanding of what stress is doing to their physiology. Second, help them see their ability to cope is not about toughness. It is about adaptability. Third, help them build habits that support recovery. Practicing mindfulness can help some patients. For others, it might be boundaries, training changes, or sleep consistency. If the situation is complex, refer appropriately. Professional help is a strength, not a failure, and collaboration with a mental health professional can be exactly what a patient needs while you continue supporting nervous system performance in your lane.
Using INSiGHT Scanning Technology to Anchor Normal Stress Level Conversations in Objective Data
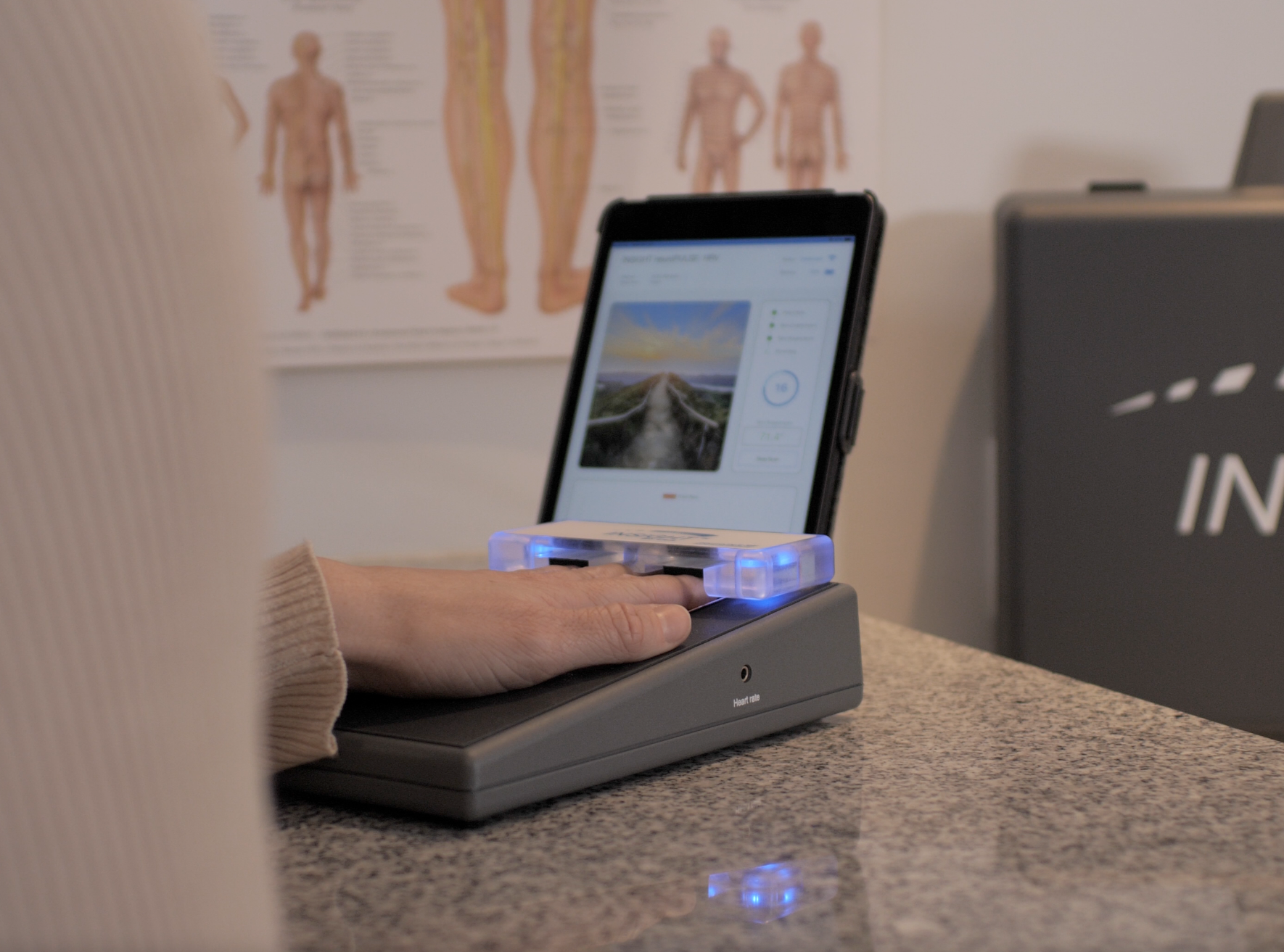
This is where chiropractors stop guessing and start leading. INSiGHT scanning technology provides objective exam data and scan reports that support chiropractors in building a care plan. The INSiGHT does not create the care plan itself. The chiropractor interprets the findings, connects them to function, and recommends next steps. When you bring this approach into a normal stress level conversation, the whole tone changes. Instead of trying to convince a patient they are under stress, you show what their nervous system status looks like today and how it is trending over time.
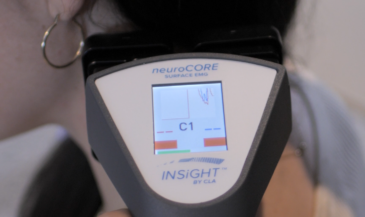
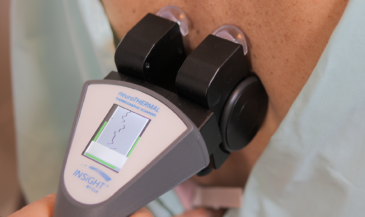
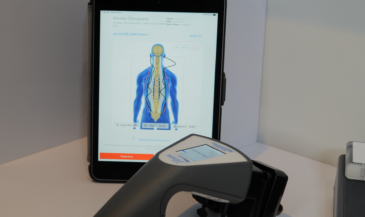
Start with neuroPULSE for HRV, because it helps you speak clearly about adaptability and recovery. You can explain whether the nervous system is spending most of its time in fight-or-flight or whether it can downshift when the day is done. Then support the bigger story with neuroTHERMAL, which provides analysis of segmental neurological distress trends, and neuroCORE sEMG, which provides analysis of neuromuscular energy output and motor tone responses. In Synapse software, those scan views become a shared reference point. Patients do not have to argue with you. They can see what is happening.
In practice flow, it can look simple. Establish baseline early. Explain that the goal is not to eliminate all stress, but to help the patient build a normal stress level that includes real recovery. Re-scan on a reasonable schedule to see whether stress becomes more manageable, whether the system is stabilizing, and whether recovery windows are improving. This is where manage stress stops being generic advice. It becomes a measurable strategy. You can still recommend ways to cope such as sleep improvements, movement, relaxation practice, and lifestyle changes, but now the patient has feedback. If their numbers improve, they trust the process. If they don’t, you adjust intelligently. This is how objective neurological scanning helps chiropractors guide care with more certainty and communicate progress in a way patients can understand.
When Normal Stress Level Starts to Look Like Recovery Again
So, what is a normal stress level in the real world? It is not a day with zero stress. It is a week where the nervous system can work, respond, and then recover. It is a system that can handle everyday stressors without staying stuck in overdrive. It is a baseline that is stable enough for the patient to feel more resilient, sleep more consistently, and show up with more margin. That is what we are really after.
Stress from time to time is normal. Stress can be positive when it is followed by restoration. The difference between good stress and bad stress is not the event itself, but the recovery that follows. If the patient’s life is demanding, help them focus on what is measurable and changeable. Help them identify what triggers your stress. Help them build routines that support recovery. Encourage them to manage your stress with habits that are realistic, not heroic. Remind them that important to manage your stress is not a moral statement. It is a biological one.
And for chiropractors, keep leading with objective clarity. Use wearables as a conversation starter, not a diagnosis. Use scanning to anchor the story. When you can show trend, the patient stops guessing. They stop debating. They start understanding. That is how normal stress level becomes a useful clinical concept, not just another phrase people throw around when they’re tired.