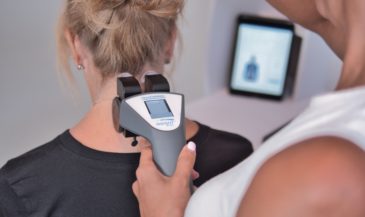
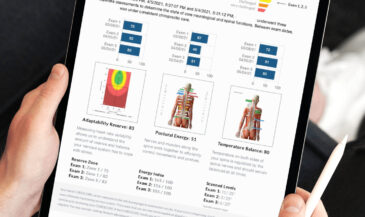
Paraspinal muscles matter because they are often the first place you can see how the nervous system is adapting. If you can make that adaptation measurable and visible, you lead with certainty instead of guesswork.
Why Paraspinal Matters in Chiropractic Practice
In chiropractic today, the paraspinal muscles are often treated like a side note: “tight on the left,” “spasm in the low back,” “guarding around L4.” Useful observations, sure. But if we stop there, we miss what those observations are trying to tell us. Paraspinal tone is frequently a protective output, and protective output is a nervous system decision.
The paraspinal muscles in the control of posture and segmental stability do more than hold you upright. They help the body decide how to distribute load, how to brace, and how to move without collapse. That is why patients with the same back pain condition can look completely different in movement. One hinges cleanly. One braces like a plank. One can twist. One cannot. Their spine-related pain might be similar, but the strategy is not.
This is also why you will see paraspinal patterns show up across the whole spine. A patient may complain about low back symptoms, but you observe altered alignment and movement from the pelvis into the thoracic spine and even the cervical spine. The body does not compartmentalize the way we label regions. It adapts globally. When you treat paraspinal as a system, your evaluation gets sharper and your communication gets simpler.
If you want a practical way to frame it for a patient or team member, use this line: the paraspinal muscles allow the spine to be stable and still move. That is the target. Not just less guarding today, but more options tomorrow.
Anatomy and Function Chiropractors Need to Know
Paraspinal is not one muscle. It is a group of muscles that run vertically along the spinal column on both sides, nested between the vertebrae and ribs, spanning from upper regions down toward the pelvis. That placement is strategic. It lets the body support the spine, fine-tune movement, and protect segments under load.
From a clinical lens, two layers matter most. First, the erector spinae muscles, including iliocostalis, longissimus, and spinalis. These are the workhorses for extension and general trunk support, and they function like a long extensor muscle system that helps maintain posture over time. Second, the deep segmental stabilizers, including multifidus and other transversospinalis fibers, provide fine control and stabilize the motion segment when the patient bends, twists, or transitions from load to movement. This is the layer that quietly decides whether a patient moves smoothly or braces through every task.
And none of this happens in isolation. Paraspinal function depends on coordination with abdominal muscles and other core muscles, the pelvis, and hip stabilizers. That is why relationships like paraspinal and psoas muscle and paraspinal and quadratus lumborum muscles show up constantly in clinical discussion. When deep stabilizers underperform, other muscles try to “save the day.” It can look like strength, but it is often compensation.
This is where the phrase hold up the spine becomes more than a metaphor. The paraspinal system is managing load, timing, and coordination while the body is moving. When you ask a patient to arch your back, rotate, or hinge, you are watching the nervous system choose a strategy. If the strategy is rigid, we do not just blame flexibility. We ask why stability is being bought with stiffness.
Learn more about INSiGHT scanning?
Fill this out and we’ll get in touch!
"*" indicates required fields
Common Paraspinal Problems Chiropractors See Every Day
Most paraspinal complaints in practice follow a familiar pattern. A patient has a back injury, a sudden flare-up, or a slow-building fatigue problem, and the next thing you see is protective guarding and reduced tolerance. Over time, repeated episodes create predictable movement habits that can turn acute events into chronic back pain. You will also see unilateral back pain patterns where one side of the paraspinal system becomes the primary stabilizer, and the patient loses symmetry and endurance.
In acute cases, you often see spasm, strain, and a clear “don’t go there” response when they try to move. In chronic cases, the more interesting story is paraspinal muscle quality. This is where research discussions around fatty infiltration of muscles become relevant. When tissue composition shifts, performance shifts. Authors will describe fat content and weakness, and they will debate how fatty infiltration of muscles affects stability, endurance, and motor control in long-standing cases. That does not mean every chronic patient has the same tissue changes, but it does mean the paraspinal story is not always solved by rest, stretching, or “just getting adjusted.”
Clinically, you will see this show up as changes in the paraspinal that alter movement and load tolerance. In the literature, you might see terms like paraspinal muscle changes, structural changes of lumbar muscles, and chronic paraspinal muscle patterns tied to low back disability and pain and disability discussions. You will also see broader concepts like damage and chronic low back and endplate damage and chronic low show up as part of chronic low back conversations. Some papers describe how changes contributed to the back and contributed to the back pain, but in daily practice, the question remains the same: can the patient stabilize, adapt, and move without bracing?
One of the most common combinations chiropractors observe is a strong-looking back with poor control. The quadratus lumborum muscles were still overactive, the lumborum muscles were still weak in endurance and coordination, and the patient is stuck in a protection loop. That is why finding the right exercise matters so much. You are not just building strength. You are restoring strategy.
And if you want a fascinating reminder of how quickly the system can change, look at back pain astronauts and what back pain astronauts experience after unloading in microgravity. It is a vivid example of how spine musculature can change when normal loading is removed. You do not need space travel to see the concept. You see it anytime a patient avoids movement long enough that their stabilizers lose endurance and their body shifts into compensation.
Assessment and Clinical Interpretation Without Guesswork
The best paraspinal assessment is layered. Start with what you can observe: posture, hinge mechanics, rotation tolerance, and how the patient transitions under load. This is the beginning of an honest assessment of back function, and it tells you whether the patient is moving with options or moving with protection. Stabilizing the spine is not just a strength question. It is a coordination question.
Then add your hands-on findings in a way that supports the story instead of replacing it. Palpation, tissue tone, and segmental motion are part of the chiropractic treatment, but they are not the whole picture. Tie them to what the patient can do and what you can document. If the patient braces through rotation, note that. If they cannot tolerate extension, note that. If their ability to move your spine is limited by guarding, note that. You are building a functional narrative, not a list of tender spots.
When imaging is available, it can add context, especially in chronic cases. MRI and CT are commonly used in research to look at the cross-sectional area of these muscles and the presence of atrophy or fatty infiltration. You will see authors discuss using the cross-sectional area as a way to quantify change, and you may see a longitudinal magnetic resonance imaging study design used to track changes over time. You may also see discussions that include lumbar intervertebral disc degeneration, degenerative lumbar findings, atrophy after posterior procedures, and anatomy of the lumbar spine as part of the broader picture. Keep the messaging steady: imaging can describe structure, but it does not directly measure symptoms.
This is where objective muscle activity data can be a practical bridge. Surface EMG helps you measure motor output patterns that can otherwise be hard to communicate. It is not a standalone diagnostic tool, and it is not a symptom meter. But it can support your assessment of back when interpreted responsibly and compared against appropriate norms. In the end, muscles are the muscles, but the nervous system decides how they fire. That is what you are tracking.
How Neurological Scanning Guides a Paraspinal-Centered Strategy
If you want paraspinal care to feel modern, precise, and easy to communicate, you need objective data. This is where neurological scanning changes the tone of the conversation. Instead of explaining everything as “tight” or “weak,” you can show patterns that explain why the patient is stuck, and you can document how those patterns change over time. That is the difference between a vague plan and a chiropractic treatment plan to strengthen function with confidence.
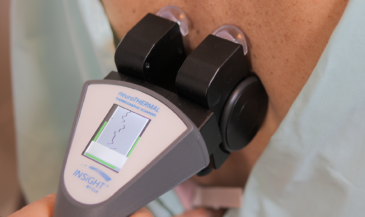
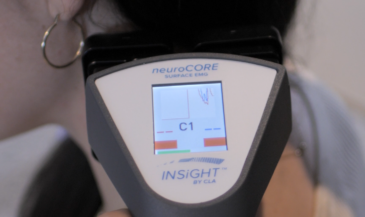
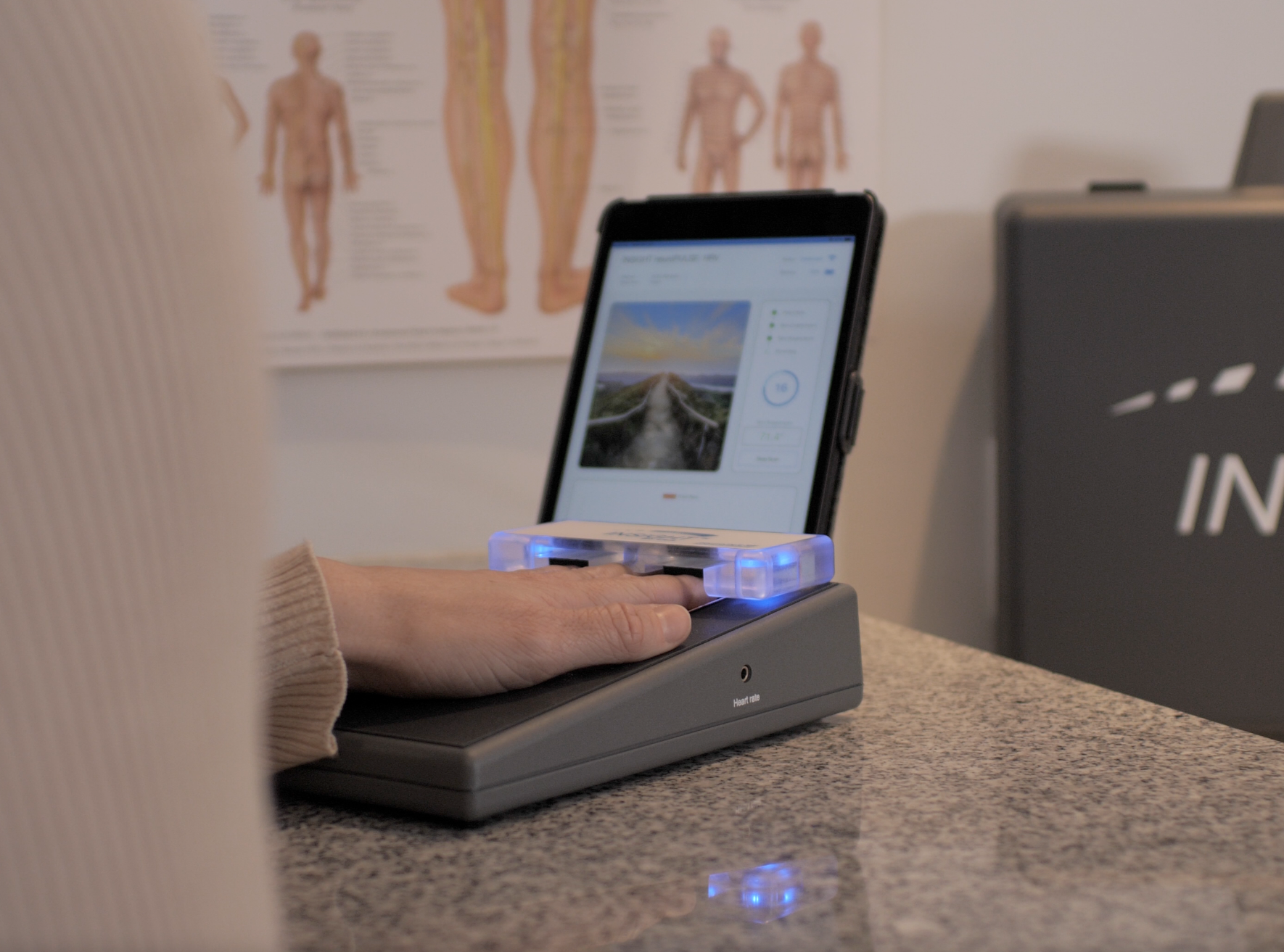
In the INSiGHT neuroTECH and Synapse software, each technology supports a different layer of the paraspinal story. neuroCORE sEMG supports the motor tone conversation. It helps you document patterns that relate to muscle weakness, asymmetry, and guarding, and it supports tracking your efforts to strengthen the paraspinal system over time. neuroTHERMAL supports a segmental stress pattern conversation, giving you a visual map that can match what you are seeing in motion. neuroPULSE HRV gives you a read on adaptability and resilience, which matters when a patient is stuck in sympathetic overdrive and cannot downshift. None of these instruments create the care plan. They provide objective exam data and reports that you interpret and use to guide decisions.
On the soft tissue side, you will also see approaches that include treating paraspinal tissue directly. That may include treatment of paraspinal muscles via manual work, and in some practices, paraspinal muscles via fascia manipulation is used to support improved movement options. You will even see phrases like muscles via fascia manipulation goes and via fascia manipulation goes along in summaries because clinicians are trying to describe sequencing. In real-world terms, the goal is coordination: fascia work supports motion, and the adjustment supports function. You may also see language like along with spinal manipulation treatment when the plan includes both components. Use what is accurate for your office and your documentation standards.
When you build the plan around capacity and measurement, you can give patients a simple path. Start with movement confidence, add control, then add endurance. Use exercises as part of the plan, not as an afterthought. This is where chiropractic recommends exercises as part of restoring stability and tolerance. You can include exercises to strengthen, a specific form of exercise early, then progress to a higher-demand type of exercise, and eventually high intensity or other type loading only when control is stable. That progression matters because strength or lack thereof changes how the body protects. And when the patient asks whether paraspinal muscles can be beneficial to focus on, you can answer clearly: yes, because critical paraspinal muscles help stabilize and adapt. The goal is the strength of these critical paraspinal stabilizers, not just soreness from a workout.
Make Paraspinal Measurable, Not Mysterious
Paraspinal care works best when it is simple, honest, and measurable. You are not trying to “fix a tight spot.” You are guiding the nervous system and the motor system back toward options. That means you respect stability, you respect endurance, and you build a plan the patient can follow. That is how you help relieve pain and also relieve back pain in a way that holds up over time.
Use practical language and stay grounded. Explain that the spine and allow movement depends on coordinated stabilizers, not just flexible tissue. Remind them that the spine as you must manage it is a system, and the whole spine adapts together. If they ask why one side keeps taking over, explain the lack thereof of your paraspinal control and the thereof of your paraspinal muscles endurance, then show them what you mean with objective data.
- Use a consistent assessment each visit so progress is visible, not assumed. If you have INSiGHT scanning tech in your practice, we use a progress report called the CORESCORE.
- Build movement confidence first, then layer in muscle exercises and progressive loading.
- Choose the lowest dose that restores control, then progress. Do not skip the basics.
- Remember the broader context: thoracic spine and cervical spine mechanics influence lumbar strategy, and neck and back patterns often travel together across the global spine. You will see authors debate an association with low outcomes, but your job is to evaluate function and capacity today.
The neuroCORE sEMG helps you document motor tone patterns and track change. neuroTHERMAL helps you visualize segmental stress patterns. neuroPULSE HRV helps you explain adaptability and resilience when neurological distress is driving protection. When patients can see that story, they follow it. When your team can see it, they communicate it. That is how you make paraspinal care feel clear, modern, and worth sticking with.