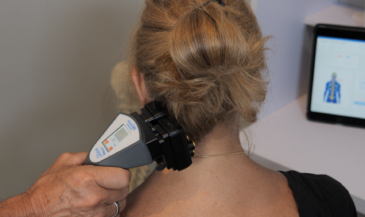
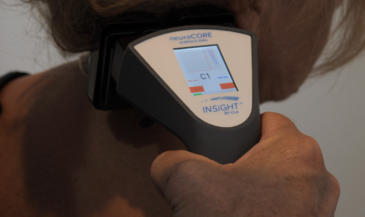
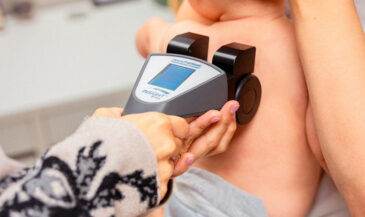
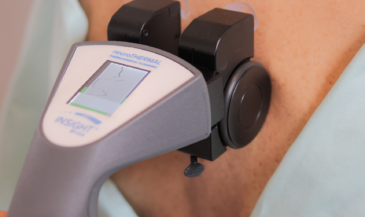
In addition to techniques of skin temperature measurement, sweat gland activity is another indicator of sympathetic function. Sympathetic stimulation causes increased sweat gland activity. Increased sweat gland activity results in less resistance to the flow of an electrical current. Therefore, sweat gland activity may be assessed by passing a small electric current through the skin to measure resistance. Terms used to describe this procedure include ESR (electrical skin resistance), GSR (galvanic skin response), and electrodermatography. Korr, Thomas and Wright (1) summarized the physiologic rationale for evaluating patterns of electrical skin resistance in humans:
1. Electrical skin resistance is related to the activity of the sweat glands.
2. Interruption or retardation of the flow of impulses over sympathetic pathways to an area causes a marked elevation of resistance in that area.
3. Stimulation of sympathetic pathways either locally or systemically lowers the resistance.
Korr and Goldstein (2) observed that segmental differences in sweat gland activity are related to segments with reduced motor reflex thresholds. Areas of reduced skin resistance were often hyperesthetic. It was concluded that in segments with chronically reduced motor reflex thresholds, at least some of the preganglionic sympathetic neurons of the same segment are also maintained in a state of facilitation (lowered thresholds).
The results of investigations employing skin resistance methods to evaluate manifestations of visceral disease or segmental dysfunction have yielded equivocal results. This may be due, in part, to variations in technique and interpretation.
Korr (3) reported the results of a preliminary investigation to determine if paraspinal skin resistance patterns were related to visceral disease. Two classes of patients were evaluated. One group of patients had a history of myocardial infarction, and demonstrated low resistance areas over 2 or more of the upper 4 thoracic vertebrae. In one patient, such areas were observed three weeks prior to coronary occlusion. The second group of patients had duodenal cap ulcers. These individuals had low resistance areas at the T5 to T8 areas.
In a later work, Korr (4) stated that after examining hundreds of patients, “each had a rather characteristic pattern that remained fairly constant; the size of the areas might vary but the segmental distributions retained the individual’s characteristic pattern. We could identify the subject from his ESR — electrical skin resistance chart — almost as readily as one can from fingerprints. …Repeatedly it has been demonstrated that the distribution of low skin resistance — that is, areas of sympathetic nerve activity — correspond quite well to the actual nerve distribution of the lesioned segment in the spine.”
These conclusions are refuted by other investigators using skin resistance measurements. Bauch and Hartig (5) concluded that the electrodermatogram was unreliable as an independent or differential diagnostic method. It was concluded that due to nervous system overlap, segmental localization was imprecise and therefore not organ specific. The authors noted that the asymmetry of the conductivity between the two sides of the body was a phenomenon which could not be explained.
Plaugher et al (6) investigated the interexaminer reliability of a galvanic skin resistance device for the detection of low resistance areas along the spinal column in “relatively asymptomatic” subjects. Only modest levels of concordance were found. The authors suggest that the unevenness of data generated in certain spinal regions necessitates further investigation prior to reaching conclusions about the usefulness of this instrument in a clinical setting.
A possible explanation for these conclusions is offered by Korr (4). “You must not look for perfect correspondence between skin resistance and the distribution of the pathologic disturbance, because an area of skin which is segmentally related to a particular muscle does not necessarily overlap that muscle. With the latissimus dorsi, for example, the myofascial disturbance might be over the hip but the reflex manifestations would be in much higher dermatomes because this muscle has its innervation from the cervical part of the spinal cord.”
Ellestad et al (7) reported statistically significant changes in paraspinal skin resistance in back pain patients who received osteopathic manipulative treatment (OMT). Specifically, skin resistance decreased following OMT. The authors suggested that this may be due to a greater degree of relaxation. It was also reported that SEMG activity decreased following OMT.
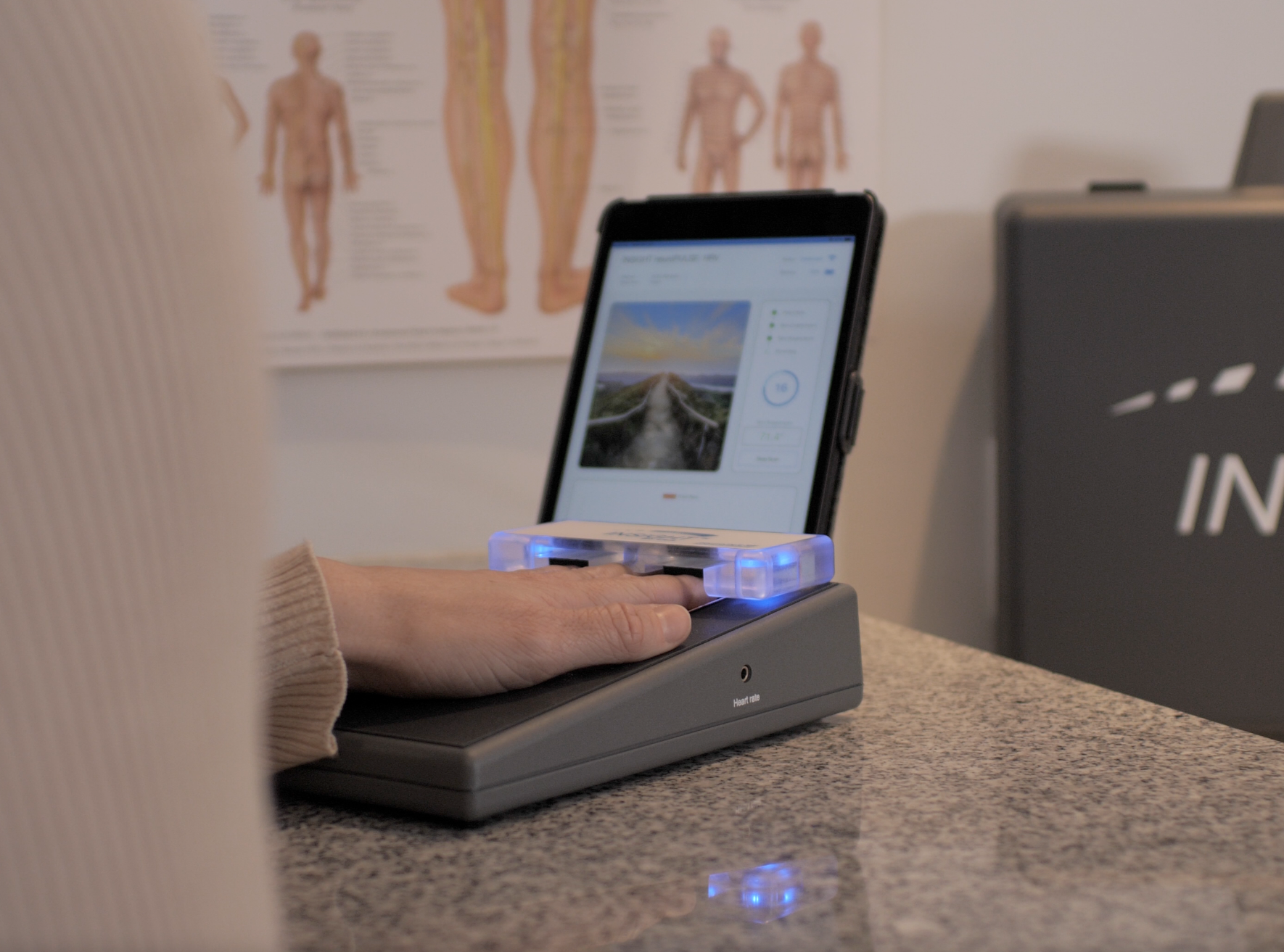
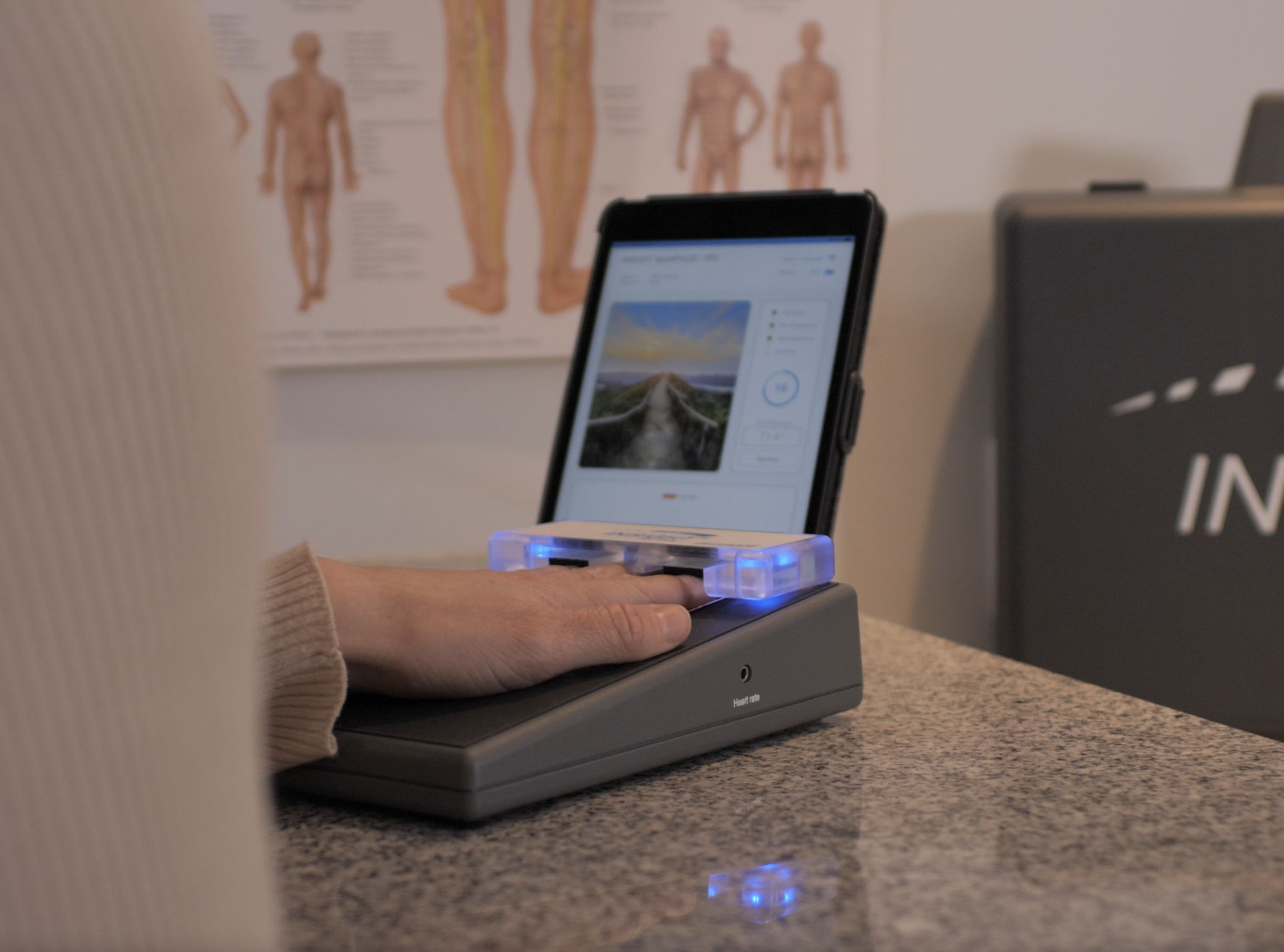
In addition to assessing segmental autonomic function, skin resistance measurements may be used as indicators of general autonomic activity. Such measurements are often taken at the fingertips. This procedure is often used in biofeedback training to teach relaxation techniques.
A small study by Giesen, Center and Leach (8) used electrodermal measurements to assess autonomic nervous system activity in hyperactive children receiving chiropractic care. Behavioral assessments were also used to evaluate outcomes. The authors concluded that chiropractic care has the potential to become an important intervention for children with hyperactivity. Because of equivocal findings, and a paucity of published research in the chiropractic literature, the acceptance of skin resistance instrumentation in general clinical practice has been limited. Additional research to explore its potential value in assessing autonomic dysfunction associated with vertebral subluxation should be encouraged.
References
1. Korr IM, Thomas PE, Wright HM: “Patterns of electrical skin resistance in man.” J Neural Transmission 1958;17:77.
2. Korr IM, Goldstein MJ: “Abstract: dermatomal autonomic activity in relation to segmental motor reflex threshold.” Federation Proceedings 1948;7:67. In: The Collected Papers of Irvin M. Korr. American Academy of Osteopathy. Indianapolis, IN. 1979. P. 22.
3. Korr IM: “Abstract: skin resistance patterns associated with visceral disease.” Federation Proceedings 1949;8:87. In: The Collected Papers of Irvin M. Korr. American Academy of Osteopathy. Indianapolis, IN. 1979. P. 23.
4. Korr IM: “The segmental nervous system as a mediator and organizer of disease processes.” The Physiologic Basis of Osteopathic Medicine. The Postgraduate Institute of Osteopathic Medicine and Surgery. 1970:73.
5. Bauch K, Hartig W: “Electrodermatographic examination of segmental sweat secretion in the diagnosis and differential diagnosis of internal diseases.” Acta Neurovegetativa 1973;30:536.
6. Plaugher G, Haas M, Doble RW Jr et al: “The interexaminer reliability of a galvanic skin response instrument.” J Manipulative Physiol Ther 1993;16(7):453.
7. Ellestad S, Nagle R, Boesler D, Kilmore M: “Electromyographic and skin resistance responses to osteopathic manipulative treatment for low-back pain.” JAOA 1988;88(8):991.
8. Giesen J, Center D, Leach R: “An evaluation of chiropractic manipulation as a treatment of hyperactivity in children.” J Manipulative Physiol Ther 1989;12:353.