By Dr. Christopher Kent
A popular childhood fable is “The Emperor’s New Clothes.” In this delightful tale, a con artist offers to tailor a suit of clothes for an insecure emperor. The confidence man assures the emperor that the proposed suit will be the finest available. In addition, the suit will posses a magical property. Only the wise will be able to behold its majesty. To a fool, the suit will be completely invisible.
For weeks the con man surrounds himself with the trappings of a skilled tailor. He pretends to spin, weave, and sew the emperor’s new suit. Finally, he summons the emperor, pretending to dress him in the wonderful new suit. The emperor, not wanting to appear a fool, extols the virtues of his expensive new garb. Following his lead, the emperor’s servants concur. No one wants to play the fool.
The emperor announces his plans to wear this magical suit of clothes in a parade. With the announcement of the parade, the people are also advised that only the wise will be able to see the new clothes. To a fool, the garments will be invisible. During the course of the parade, the people of the kingdom praise the emperor’s new clothes. All seems well until one small child announces, “The emperor is naked!” That ends the ruse, and it becomes apparent to all who the fools are.
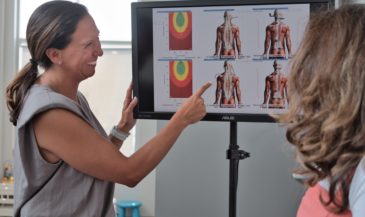
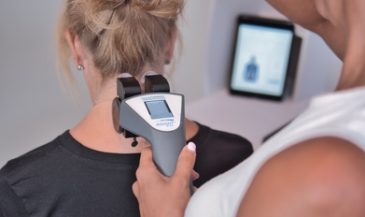
Unfortunately, the chiropractic profession has an abundance of naked emperors. These are the so-called researchers and insurance consultants who, feigning scientific objectivity, actively disparage modern chiropractic diagnostic procedures. These emperors offer glib proclamations that surface EMG, thermography, and videofluoroscopy are “investigational” procedures. As such, they seek to deny third party payment for such procedures.
The problem, of course, is their double standard. Perhaps it would be more appropriate to say their lack of any standards. For while they “trash” these new techniques, they seemingly have no problems whatever with billings for “traditional” procedures possessing far weaker scientific foundations.
They “allow” billings for office visits and examinations incorporating static palpation, motion palpation, and range of motion exams. Yet, where is the scientific documentation demonstrating the reliability, validity, sensitivity, specificity, and predictive value of these procedures?
If such evidence must be offered for surface EMG, thermography, and videofluoroscopy, why isn’t the same standard applied to palpation, range of motion, orthopedic/neurological examination procedures, muscle tests, and similar techniques that are reimbursed without question? Where are the references to support their pompous proclamations?
Like the emperor’s clothes, there aren’t any.
Surprisingly, there appears to be an inverse relationship between the concentration of vitriol cast by these naked emperors and the scientific track record of the procedure in question. Realizing that when you sling mud, you invariably lose ground, I propose an alternative — establishing criteria and reviewing the literature.
Let’s look at a popular diagnostic technique that has not incurred the wrath of the naked emperors and see how it fares when subjected to critical scrutiny.
Palpation
Several insurance consultants have suggested (although they were wise not to do so in print) that palpation is “as good as” paraspinal EMG scanning for the assessment of paraspinal muscle changes. One we spoke with even suggested that palpation is “the gold standard” of chiropractic analysis.
A brief review of the literature will demonstrate that we may well be dealing in fool’s gold. For while palpation may be highly valued by individual practitioners, the literature indicates motion palpation of the spine demonstrates marginal-to-no reliability. [1-7]
Of static palpation, Haas noted: “Currently there are no studies to confirm or refute the reliability of static palpatory procedures.” [8]
Amazingly, we have yet to hear of any naked emperor attempting to deny reimbursement for examinations which include palpation, or for treatment rendered as a result of palpatory findings. Nor have we heard anyone claim that palpation is “investigational” and should not be in general clinical usage.
Now let’s contrast these studies with those relating to surface electrode EMG.
Spector conducted a study to determine the reliability of surface electrode paraspinal EMG. Results of the study yielded correlation coefficients ranging from 0.73 to 0.97. [9]
Thompson et al of the Mayo Clinic found EMG scanning techniques correlates highly with attached electrode technique. [10]
Cram reported a mean reliability coefficient of 0.83 for surface EMG scanning. [11]
Komi and Buskirk found that the test-retest reliability of surface electrode EMG was superior to that of inserted electrode technique. The average test/retest reliability for surface electrodes was 0.88, compared to 0.62 for inserted electrode EMG. [12]
“So what if it’s reliable! What does it mean?,” shrieked an emperor at a recent seminar.
Cobb et al studied spasm of the wrist extensor and paravertebral muscles. They found that needle electrodes showed no evidence of electrical activity, while surface electrodes revealed even mild muscle spasm. [13]
Even more interesting is the work of Shambaugh who compared surface paraspinal EMG potentials in patients receiving chiropractic adjustments with controls. Shambaugh concluded, “Results of this study show that significant changes in muscle electrical activity occur as a consequence of adjusting.” [14]
Ellestad et al found that surface paraspinal EMG activity decreased in patients following spinal manipulation. Such changes were not observed in the control subjects. [15]
Protocols and normative data have been published in a refereed chiropractic journal, enabling chiropractors to compare a patient under examination with a normative population. [16]
The question I pose to the emperors is simple: How many techniques in chiropractic meet the following criteria?
1. Very good-to-excellent reliability according to studies conducted both within the chiropractic profession and by investigators in other professions.
2. Protocols and normative data available in refereed, peer-reviewed literature.
3. Specific indications for the test published in refereed, peer-reviewed literature.
4. Completely non-invasive. No contraindications. No radiation. No signal introduced into the body.
5. Taught under the aegis of accredited chiropractic colleges.
6. Shown through studies published in refereed, peer-reviewed journals to change with adjustment or manipulation, yet not change significantly in controls.
The most ridiculous argument to date came from an emperor working as an insurance prostitute. He said, “Chiropractors did all right before thermography, fluoroscopy, and EMG. Why do they need them now?” My response was swift: “M.D.s did just fine before antibiotics, insulin, and MRI. Why do they need them now?”
When quantitative assessment of urinary glucose become available, some 19th century physicians were resistant. “Who needs it? I can taste the urine. If it’s sweet, the patient is diabetic and will die.” Yet, even before the availability of insulin, dietary management and quantitative monitoring of urine and blood glucose prolonged many lives.
Quantitative evaluation of paraspinal muscle function as a patient progresses through a course of chiropractic care objectifies clinical outcome assessment.
The “Chiropractor’s Oath” which we took on graduation day included a statement that “I will keep an open mind regarding the progress of my profession.” Sadly, the oath did not include a pledge to refrain from keeping secret “proprietary” insurance guidelines, claim cutting, interfering with other doctor-patient relationships, or insurance prostitution in general.
Perhaps some of the emperors went to colleges which did not require such an oath. And, of course, there are a few vocal emperors who, while not chiropractors, stand ready to judge chiropractic diagnostic techniques.
The proclamations of the emperors remind me of a certain pot calling a kettle black. As I recall, it might have been a cracked pot at that. They can’t have it both ways. They can’t set a double standard. They can’t impose a more burdensome standard on one technique than another.
If they brand surface EMG “investigational,” they will be forced to admit that every other chiropractic technique is “investigational” as well. If they “throw out” surface EMG, they must “throw out” virtually all chiropractic procedures. This also holds true for much of medicine and most of surgery.
So, next time a naked emperor streaks into your practice pontificating and propagating poppycock, don’t feel shy about calling his bluff. He can’t see the suit of clothes, either. But fear not. He’ll soon be facing a brand new suit — this time in a court of law.
References
1. Keating J: “Inter-examiner reliability of motion palpation of the lumbar spine: a review of the quantitative literature.” Proceedings of the Scientific Symposium on Spinal Biomechanics. International Chiropractors Association. May 19-21, 1989.
2. Cassidy J, Potter G: “Motion examination of the lumbar spine.” JMPT 2(3):151, 1979.
3. Gonella C, Paris S, Kutner M: “Reliability in evaluating passive intervertebral motion.” Phys Ther 62(4):435, 1982.
4. Bergstrom E, Courtis G: “An inter-and intra-examiner reliability study of motion palpation in lateral flexion in the seated position.” Euro J Chiro 34:121, 1986.
5. Love R, Brodeur R: “Inter-and intra-examiner reliability of motion palpation for the thoracolumbar spine.” JMPT 10(1):1, 1987.
6. Jull G, Bullock M: “A motion profile of the lumbar spine in an aging population assessed by manual examination.” Physiotherapy Practice 3:70, 1987.
7. Boline P, Keating J, Brist J, Denver G: “Inter-examiner reliability of palpatory evaluations of the lumbar spine.” Am J Chiro Med 1(1):5, 1988.
8. Haas M: “Reliability in the chiropractic literature: a critical review.” Proceedings of the 1990 International Conference on Spinal Manipulation. May 11-12, 1990.
9. Spector B: “Surface electromyography as a model for the development of standardized procedures and reliability testing.” JMPT 2(4):214, 1979.
10. Thompson J, Erickson R, Offord K: “EMG muscle scanning: stability of hand-held electrodes.” Biofeedback Self Regul 14(1):55, 1989.
11. Cram J: “Clinical EMG: Muscle Scanning for Surface Recording.” Biofeedback Institute of Seattle. Seattle, WA, 1986.
12. Komi P, Buskirk E: “Reproducibility of electromyographic measurements with inserted wire electrodes and surface electrodes.” Electromyography 10:357, 1970.
13. Cobb C, deVries H, Urban R, Leukens C, Bagg R: “Electrical activity in muscle pain.” Am J Phys Med 54(2):80, 1975.
14. Shambaugh P: “Changes in electrical activity in muscles resulting from chiropractic adjustment: a pilot study.” JMPT 10(6):300, 1987.
15. Ellestad S, Nagle R, Boesler D, Kilmore M: “Electromyographic and skin resistance responses to osteopathic manipulative treatment for low back pain.” JAOA 88(8):991, 1988.
16. Kent C, Gentempo P: “Protocols and normative data for paraspinal EMG scanning in chiropractic practice. Chiropractic: The Journal of Research and Clinical Investigation. 6(3):64, 1990.