By Dr. Christopher Kent
Traditional chiropractic analysis includes examination of the paravertebral tissues for “taut and tender” muscle fibres. D.D. Palmer expressed the relationship between “tone” and the dynamics of health and disease: “Life is an expression of tone. Tone is the normal degree of nerve tension. Tone is expressed in function by normal elasticity, strength, and excitability…the cause of disease is any variation in tone.” [1]
Evaluation of paraspinal muscle dysfunction is generally accepted as a method for assessment of the vertebral subluxation complex. [2,3]
Pathophysiology
The role of articular mechanoreceptors in producing aberrant afferent input to the CNS has been explored by other investigators. In the context of SEMG assessment of paraspinal muscle activity, it has been suggested that articular mechanoreceptors and muscle spindles are activated during adjustment or manipulation. [4,5]
This is felt to result in reflex inhibition of spastic muscles in the affected area. This increased sensory input is also believed to result in reduced transmission of nociceptive signals, resulting is decreased pain perception. Type II mechanoreceptors are dynamic, low threshold, and rapidly adapting. These mechanoreceptors fire impulses of less than 500 milliseconds in duration at the onset of tension changes in the joint capsule. [6,7]
Experimental evidence demonstrates that type II articular receptor reflex responses produce changes in the tone of associated muscles when the joint is moved. These reflex changes may be excitatory or inhibitory. It has been shown experimentally that the application of fast manipulative thrusts to the thoracic spine resulted a surface EMG response in the muscles of the contralateral side. However, the application of slow, gradual forces showed a gradual increase in the SEMG activity in all the muscles as the force increased. [8]
Murphy summarized the neurological pathways associated with the maintenance of background postural tone: “Weight bearing disc and mechanoreceptor functional integrity regulates and drives background postural neurologic information and function (muscular) through the unconscious mechanoreception anterior and posterior spinocerebellar tract, cerebellum, vestibular nuclei, descending medial longitudinal fasciculus (medial and lateral vestibulospinal tracts), regulatory anterior horn cell pathway.” [9]
The anterior horn cells provide motor output which travels via motor nerves to muscle fibres. Muscle fibres may be functionally classified as fast twitch and slow twitch fibres. The fast twitch fibres control phasic or fast ballistic movements. Slow twitch fibres are responsible for maintaining tonic postural support. [10]
However, the erector spinae muscles present some unique histological and physiological characteristics.
One unusual characteristic is that the slow twitch (Type I) fibres are larger in cross section than the fast twitch (Type II) fibres. The large fibres may be recruited at lower forces than the smaller fibres, which is an unusual recruitment pattern. Furthermore, the erector spinae muscles are composed of separately innervated, independently contracting discrete muscle fascicles. The erector spinae muscles rarely shorten beyond their length in the upright standing position. These factors must be considered when assessing SEMG patterns in the erector spinae. [11]
Bullock-Saxton, Janda, and Bullock have used SEMG techniques to assess subconscious and automatic responses in muscle activation patterns. [12,13]
Janda has suggested that good function of peripheral structures, good muscle balance, and activation of the spinocerello- vestibular circuits facilitates the most important afferent pathways and centers. [14]
Whatmore and Kohi described an important neurophysiologic factor in functional disorders which they termed “dysponesis.” Dysponesis refers to a reversible physiopathologic state consisting of errors in energy expenditure, which are capable of producing functional disorders. Dysponesis consists mainly of covert errors in action potential output from the motor and premotor areas of the cortex and the consequences of that output. These neurophysiological reactions may result from responses to environmental events, bodily sensations, and emotions. The resulting aberrant muscle activity may be evaluated using surface electrode techniques. [15]
Paraspinal scanning technique
Protocols and normative data for paraspinal EMG scanning have been published in the refereed literature. [16]
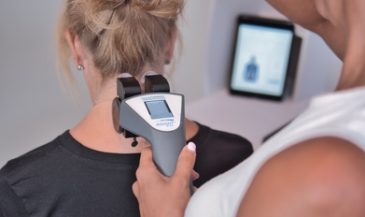
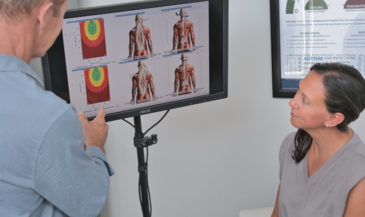
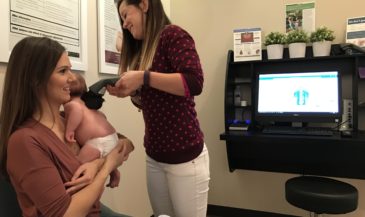
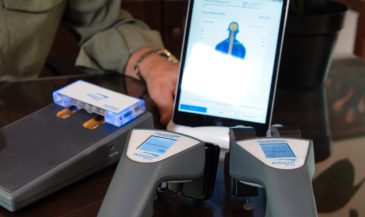
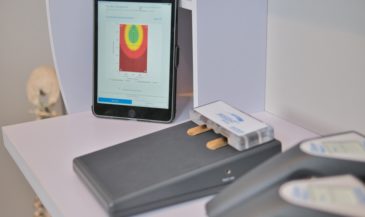
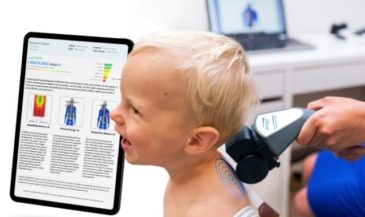
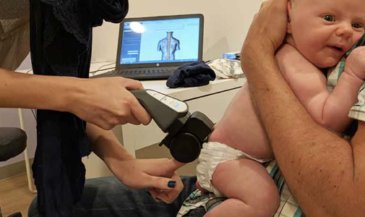
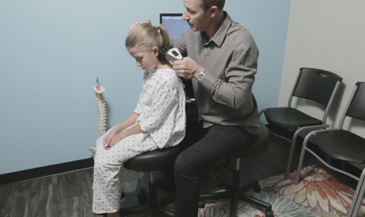
Hand-held electrodes are applied to the skin of the patient overlying the spine at 15 paired sites. EMG signals are measured in microvolts (millionths of a volt). A computer analyses these signals, and compares them to a normative data base. In the interpretation of SEMG scans, three factors are considered:
1. Amplitude. This refers to the signal level in
microvolts. The higher the signal level, the
greater the extent of the paraspinal muscle activity. By comparing these readings to a normative data
base, elevated or decreased signals can be identified.
2. Symmetry. This refers to a comparison of the left side to the right side. [17]
3. Frequency shift. Fatigued muscle exhibits a lower mean or median frequency than non-fatigued muscle. [18]
Paraspinal EMG scans, taken in concert with other examination findings, may be helpful in determining the following:
*** Asymmetrical contraction
*** Areas of muscle splinting
*** Severity of the condition
*** Aberrant recruitment patterns
*** Dysponesis
*** Responses to dysafferentation
*** Response to chiropractic adjustment
Construct validity
In the absence of a “gold standard” for assessment of the muscular dysfunction associated with the vertebral subluxation complex, the clinical utility of the procedure may be evaluated by determining the ability of the test to perform up to the standards predicted by a theoretical model or construct. [19]
In the case of SEMG, the assumption is made that significant changes in SEMG activity will occur following chiropractic adjustment, and that significant changes will not be observed in controls.
Shambaugh conducted a controlled study where surface electrodes were used to record paraspinal EMG activity pre- and post- chiropractic adjustment. Shambaugh concluded, “Results of this study show that significant changes in muscle electrical activity occur as a consequence of adjusting.” [20]
In the osteopathic literature, Ellestad et al conducted a controlled study which found that paraspinal EMG activity decreased in patients following osteopathic manipulation. [21]
Such changes were not observed in controls in either study. Therefore, these studies support the construct validity of paraspinal SEMG as an outcome assessment for chiropractic adjustment.
Conclusion
Paraspinal EMG scanning is a reliable tool for the quantitative assessment of paraspinal muscle activity. Altered paraspinal muscle activity is a generally accepted manifestation of vertebral subluxation complex. Paraspinal EMG scanning may be effectively used as an outcome assessment for chiropractic care.
References
1. Palmer D: “The Chiropractor’s Adjustor,” Portland, OR. Portland Publishing House, 1910.
2. Janse J, Houser RH, Wells BF: “Chiropractic Principles and Technic.” National College of Chiropractic. Chicago, IL. 1947 (reprinted 1978).
3. Schafer RC: “Basic Chiropractic Procedural Manual.” American Chiropractic Association. Arlington, VA. 1984.
4. Gillette RG: “A speculative argument for the coactivation of diverse somatic receptor populations by forceful chiropractic adjustments.” Man Med 1987;3:1.
5. Zusman M: “Spinal manipulative therapy: review of some proposed mechanisms, and a new hypothesis.” Aust J Physiother 1986;32:89.
6. Wyke B: “The neurology of joints.” Ann R Coll Surg (Br) 1967:25.
7. Wyke B: “Neurology of the cervical spinal joints.” Physiother 1979;65:72.
8. Suter E, Herzog W, Conway PJ, Zhang YT: “Reflex response associated with manipulative treatment of the thoracic spine.” JNMS 1994;2(3):124.
9. Murphy DJ: “Neurogenic posture.” Am J of Clinical Chiropractic 1995;5(1):16.
10. Cram J: “EMG muscle scanning and diagnostic manual for surface recordings.” In Cram J (ed) “Clinical EMG for Surface Recordings: Volume 2.” Clinical Resources. Nevada City, CA. 1990.
11. Dolan P, Mannion AF, Adams MA: “Fatigue of the erector spinae muscles. A quantitative assessment using frequency banding of the surface electromyography signal.” Spine 1995;20(2):149.
12. Bullock-Saxton J, Janda V, Bullock M: “Reflex activation of gluteal muscles in walking: an approach to restoration of muscle function patients with low back pain.” Spine 1993;18(6):704.
13. Janda V: “Differential diagnosis of muscle tone in respect to inhibitory techniques.” Man Med 1989;4(3):96.
14. Janda V: “Treatment of chronic back pain.” Man Med 1992;6(5):166.
15. Whatmore GB, Kohi DR: “Dysponesis: a neurophysiologic factor in functional disorders.” Behav Sci 1968;13(2):102.
16. Kent C, Gentempo P: “Protocols and normative data for paraspinal EMG scanning in chiropractic practice.” Chiropractic Oct 1990 6(3):64.
17. Gentempo P, Kent C: “The role of paraspinal EMG scanning in managing the vertebral subluxation complex.” The American Chiropractor 1990 Mar page 7.
18. Mayer TG, Kondraske G, Mooney V, et al: “Lumbar myoelectric spectral analysis for endurance assessment. A comparison of normals with deconditioned patients.” Spine 1989;14:986.
19. Patrick DL, Deyo RA: “Generic and disease-specific measures in assessing health status and quality of life.” Med Care 1989 Mar; 27(3 Suppl):S217.
20. Shambaugh P: “Changes in electrical activity in muscles resulting from chiropractic adjustment: a pilot study.” JMPT Dec 1987 10(6):300.
21. Ellestad S, Nagle R, Boesler D, Kilmore M: “Electromyographic and skin resistance responses to osteopathic manipulative treatment for low-back pain.” JAOA 1988;88(8):991.