By Dr. Christopher Kent
Hippocrates stated: “Should one part of the body be hotter or colder than the rest, then disease is present in that part.”[1] Since then, significant advances have been made in our understanding of the relationship between the dynamics of health and alterations in temperature.
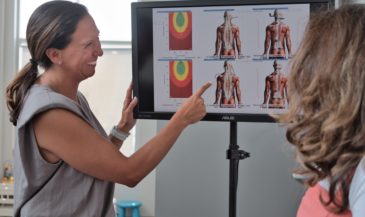
The chiropractic profession may be justly proud of being pioneers in relating altered skin temperature patterns along the spine to altered neurological function.
Dossa Evins, an engineer-turned-chiropractor, collaborated with B.J. Palmer to produce the neurocalometer in 1924.[2] The neurocalometer (NCM) is composed of two sets of thermocouples and a sensitive galvanometer. By placing the thermocouples in probes which straddle the spine, imbalances in skin temperature at like points may be detected. Later, the capability of recording these temperature differences on a strip chart was added. The instrument with the strip chart recorder was termed the neurocalograph.[3]
There are two principal systems for interpreting paraspinal skin temperature changes associated with vertebral subluxation. These are the “break system” and the “pattern system.” A break is a sharp deflection of the meter needle as the instrument glides along the skin. The level of the break is thought to be the probable level of subluxation.[4]
In the pattern system, the chiropractor compares consecutive readings acquired prior to the administration of an adjustment. If the readings demonstrate a consistent pattern, nerve interference is suggested.
Miller stated: “Persons free of neurological interference tend to display skin temperature readings which continually change, but when the vertebral subluxation and interference to normal neurological function appear on the scene, these changing differentials become static. They no longer display normal adaptability, and at this time the patients said to be ‘in pattern’.”[5]
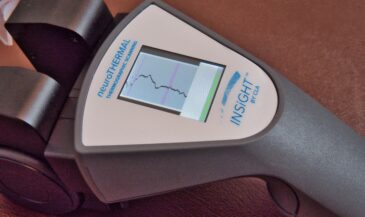
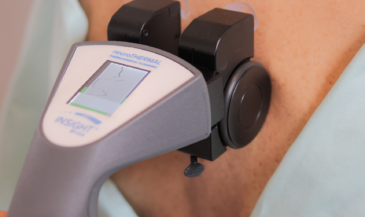
A different rationale is applied to interpreting the findings of single probe instruments, such as the dermathermograph (DTG). Cold readings, indicating vasoconstriction, are considered clinically significant. However, the regions of vasoconstriction do not necessarily indicate the level of subluxation.
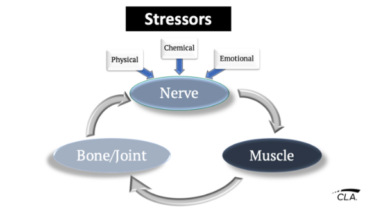
Korr developed the concept of segmental facilitation, where excess sympathetic stimulation may cause vasoconstriction of the arterioles in the skin.[6]
Stillwagon noted that after a sensory neuron synapses with the sympathetic nervous system, pre-ganglionic sympathetic fibers can ascend or descend several levels before producing a vasomotor response. Vasoconstriction may also occur as a result of sympathetic responses to recurrent meningeal nerve irritation.[7]
Acute subluxations may produce the opposite response, vasodilation. The mechanisms involved may include neuroactive substances such as histamine and prostoglandins, and antidromic stimulation of dorsal roots resulting in the release of substance P, causing vasodilation.[8]
Today, there is strong support in the scientific literature for the use of skin temperature measurement to assess sympathetic nerve function.
Uematsu et al measured the temperature differences obtained by measuring 40 matched regions of the body surface in 90 healthy subjects. They concluded, “These values can be used as a standard in assessment of sympathetic nerve function, and the degree of asymmetry is a quantifiable indicator of dysfunction.”[9]
Skin temperature instrumentation is a valuable tool for the subluxation-based chiropractor. Because the autonomic system controls organs and glands as well as blood vessels, assessment of autonomic function is important to the chiropractor concerned with the whole-body implications of the vertebral subluxation. An instrumentation examination is often an excellent place to open a dialogue with the patient concerning the whole person consequences of the subluxation.
Collection and analysis of paraspinal skin temperature data has been simplified and rendered more accurate with the availability of computer based instrumentation.
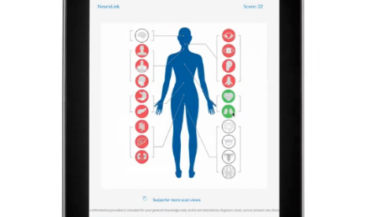
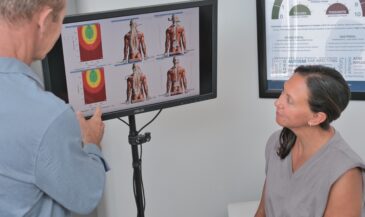
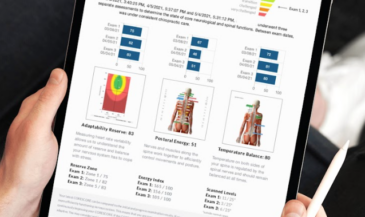
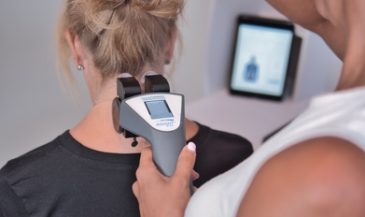
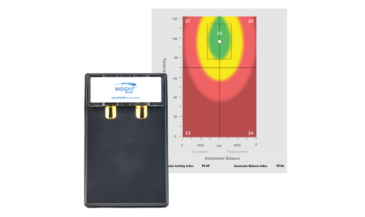
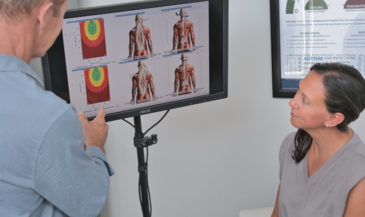
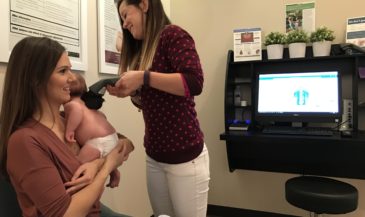
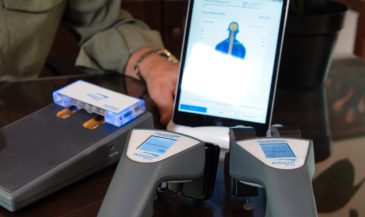
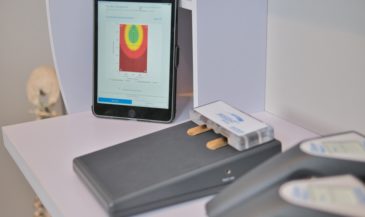
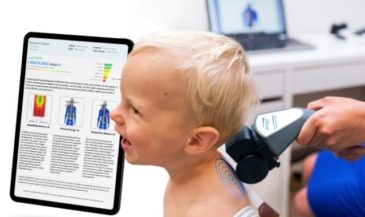
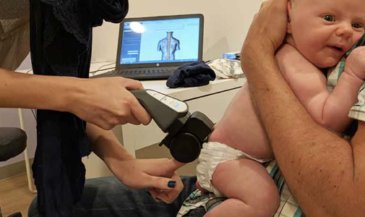
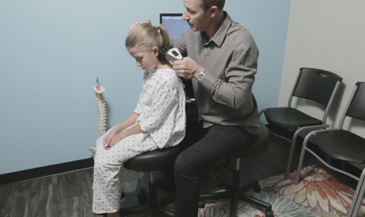
For example, the Insight Subluxation Station is an integrated platform which provides four channels of surface EMG, two channels of infrared thermometry, and an electronic inclinometer. The infrared sensors permit rapid and accurate skin temperature measurement. Once the readings are taken, the computer can supply NCM or DTG type graphics.
Furthermore, the readings of the patient can be compared to the database published in the Journal of Neurosurgery, and the number of standard deviations from these values displayed.
Instrumentation provides the chiropractor with a rapid, cost effective, objective look at nervous system function. It provides both the doctor and the patient with hard data upon which to base chiropractic management. This liberates the clinician from the symptom-chasing merry-go-round that encumbers many chiropractic practices.
To many chiropractors and patients, nerve interference is an elusive concept. With today’s technology, manifestations of nerve interference can be measured objectively and communicated effectively.
References
1. Adams F (translator): “The Genuine Works of Hippocrates.” Baltimore, MD. Williams and Wilkins. 1939.
2. Keating JC: “Introducing the Neurocalometer: a view from the Fountain Head.” Journal of the CCA (Sept 1991) 35(3):165.
3. Kent C, Gentempo P: “Instrumentation and imaging in chiropractic: a centennial retrospective.” Today’s Chiropractic (January/February 1995) 24(1):32.
4. Herbst RW: “Gonstead Chiropractic Science and Art.” Mt. Horeb, WI. Sci-Chi Publications. 1968.
5. Miller JL: “Skin temperature differential analysis.” International Review of Chiropractic Science (1964) 1(1):41.
6. Peterson B (ed): “The Collected Works of Irvin M. Korr.” American Academy of Osteopathy. 1979.
7. Stillwagon G, Stillwagon K: “Early observations of the Visi-Therm.” Today’s Chiropractic (1985) 14(6):38.
8. Kyneur JS, Bolton SP: “Chiropractic instrumentation: an update for the ’90s.” Chiropractic Journal of Australia (Sept 1991) 21(3):82.
9. Uematsu S, Edwin D, Jankel WR, et al: “Quantification of thermal asymmetry.” J Neurosurg (Oct 1988) 69:552.