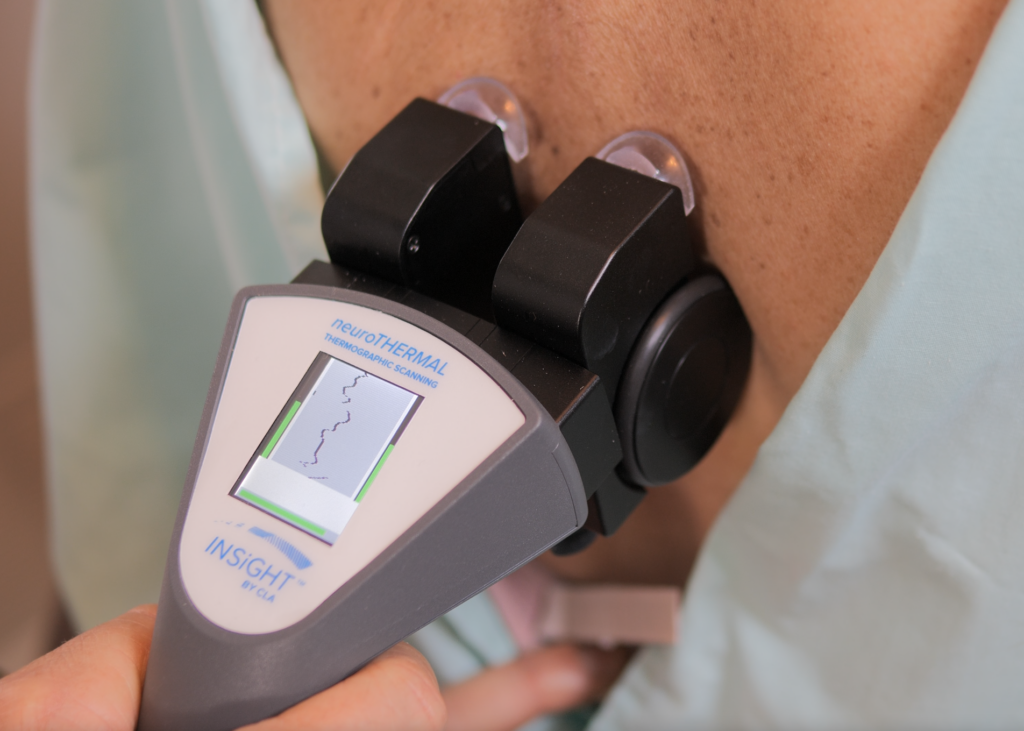
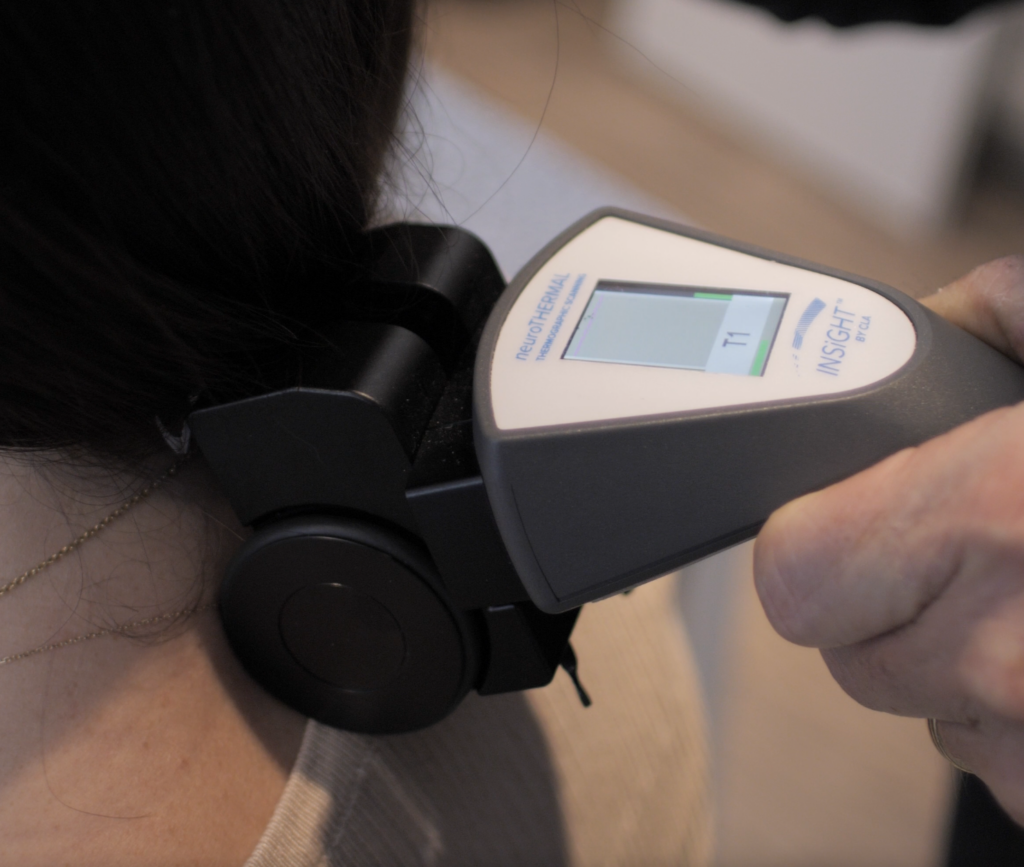
Surface electromyography has a funny way of cutting through noise in an exam. A patient can walk in with a dozen symptoms that fluctuate, a posture that “looks fine,” and a story that sounds complicated. Then you run surface electromyography, and in a moment the body tells you something simple: how hard the nervous system is working to manage gravity.
In chiropractic, electromyography is not about diagnosing muscle disease. It is about seeing motor tone, balance, and efficiency in a way that is objective and repeatable. A surface EMG scan gives you a practical look at neuromuscular control, and that makes it one of the most valuable neurological scanning tools in a modern, neurologically focused practice. When you use sEMG correctly, you move from opinions to patterns, from guesswork to real exam data, and from symptom-chasing to nervous system performance.
When patients see their surface electromyography pattern in scan views and in scan reports, you can feel the shift. They stop thinking you are only working on a joint or a single spinal region and start understanding the “why” behind the care plan. That is what objective scanning is supposed to do. It makes the invisible visible, and it gives both doctor and patient something solid to build on.
What Surface Electromyography Is and Why It Matters in Chiropractic
Let’s define it clearly. Electromyography is the process of measuring the electrical activity associated with neuromuscular function. In chiropractic, surface electromyography focuses on the paraspinal muscles because they are the daily workhorses of posture, stability, and movement coordination. Surface EMG is non-invasive. It uses a surface electrode to detect the electrical output of muscle activity through the skin surface. That means the scan is comfortable, efficient, and appropriate for patients across the life cycle.
It is also important to name what surface electromyography is not. Chiropractic surface electromyography is not the same as intramuscular EMG. Intramuscular EMG is a needle-based test used in medical settings to evaluate certain degenerative neuromuscular and nerve conduction conditions. Chiropractic SEMG is used to evaluate patterns of neuromuscular tone and organization related to neurological interference, compensatory reactions and postural tension. Surface EMG and intramuscular EMG ask different questions, and they are used for different clinical goals.
Why does this matter? Because the motor system is often where compensation shows up first. Before a person can articulate what they feel, the body is already adapting. Surface electromyography helps you see those adaptations. It gives you objective insight into whether the spinal postures are organized or scattered, balanced or biased, efficient or expensive. In practical terms, it supports the use of surface electromyography as a foundational scan for baseline exams and progress evaluations.
In many practices, this is the scan that changes the conversation. When a chiropractor can point to a clear electromyography pattern and say, “Here is where your nervous system is overworking, and here is where it is under-recruiting,” the patient understands the purpose of ongoing care. That clarity does not come from fear. It comes from visible, reproducible scan data.
The Neurological Science Behind Surface EMG Scanning
Surface electromyography is a straightforward idea with a sophisticated foundation. The nervous system communicates with muscle through electrical impulses. Those impulses originate at the motor unit, which is the motor neuron and the muscle fibers it controls. When that motor neuron fires, it generates an action potential. The combined output of many motor unit firings becomes the myoelectric signal we can detect at the surface of the body. In other words, surface EMG is capturing a biological signal that reflects neuromuscular control.
Because the scan is gathered at the surface of the skin, we are measuring a summation of activity rather than isolating deep structures. That is the clinical beauty of SEMG in chiropractic. We are not chasing a single muscle fiber. We are assessing how the spinal system is behaving as a coordinated unit. This is why the term surface myoelectric shows up in research discussions. The scan reflects myoelectric potentials with surface electrodes, and those signals are influenced by the tissue layers between muscle and sensor.
That brings us to what makes results trustworthy: signal acquisition and consistency. A clean sEMG signal depends on stable electrode contact and a repeatable scanning protocol. EMG electrodes need a reliable interface with the skin surface, and the electrode surface should be placed consistently from scan to scan. The best practices are not complicated, but they are important: consistent posture, consistent scan points, and consistent setup. This improves signal quality and makes it far easier to compare recordings over time. It also helps the chiropractor interpret trends rather than reacting to small fluctuations.
A few physiological realities are worth remembering. Subcutaneous fat on myoelectric signal transmission can reduce amplitude, meaning fat on myoelectric signal amplitude can dampen the raw signal reaching the sensor. That is not a flaw. It is simply part of interpreting a surface measurement. Chiropractic interpretation focuses less on isolated amplitude and more on symmetry, distribution, and pattern organization. When the scan is collected consistently, electromyography becomes a reliable tool for tracking change in neuromuscular organization under care.
Clinical Interpretation of Surface Electromyography in Chiropractic Practice
Now we get to the part that matters most: what to do with the scan. Surface electromyography becomes clinically meaningful when you interpret it as a pattern rather than a point. In chiropractic SEMG, we are typically evaluating whether the system is firing high, running low, or running unevenly. The most common interpretation categories include hypertonic output, hypotonic output, asymmetry, and disorganized distribution. These patterns reflect how the nervous system is managing stability, and reacting to the gravitational load.
Here is a practical way to think about it. When the motor system is compensating, it spends extra energy to do simple things. It is expensive to manage gravity. In that context, surface EMG amplitude is not about “tight muscles.” It is the nervous system paying a higher cost to maintain posture. A global pattern of elevated output suggests increased effort. A scattered pattern suggests poor coordination between spinal regions. A consistent left-right imbalance suggests the body is not sharing load well and is relying on biased strategies for stability.
Most chiropractic electromyography systems present this data visually, often with color coding relative to a normative reference. Those EMG images help patients understand what the chiropractor is describing. It is also where you anchor your progress conversation. Symptoms fluctuate. Scan patterns tend to change more gradually. When you compare recordings, you can show whether the system is organizing toward efficiency. In that way, EMG data provides proof your care is making a difference without relying on the patient’s day-to-day symptom report.
To keep interpretation consistent, focus on these essentials:
- Overall output: is the system overworking or conserving energy appropriately?
- Symmetry: are left and right sides balanced, or is one side consistently driving?
- Pattern: is the spine organized top-to-bottom, or is the activity scattered?
- Segment relationships: are there clusters of abnormal activity that suggest neurological interference patterns?
From a workflow standpoint, this is why recording matters. When the recording of emg signals is standardized, trends become obvious. That is also where a good EMG recording protocol protects you from overinterpreting noise. You are not trying to make surface electromyography sound like electrical and electronics engineering. You are trying to make it clinically useful, repeatable, and clear.
Surface EMG as Part of a Neurological Scanning Model
Surface electromyography is powerful on its own, but it becomes far more valuable when it is part of a broader neurological scanning model. In neurologically focused chiropractic, the goal is not a single snapshot. The goal is a profile. Surface EMG gives insight into the motor system. Other scans help evaluate autonomic regulation and adaptability. When those data points are viewed together, chiropractors stop “chasing segments” and start leading with neurological clarity.
This is where the use of surface EMG becomes strategic. You baseline the patient, then you re-scan at intentional intervals to see how the nervous system is adapting. The scan is not there to react to every symptom fluctuation. It is there to track neurological organization over time. This is especially important with kids, athletes, and stressed-out adults who normalize neurological distress. Scanning gives you a neutral reference point. It also makes your report of findings more consistent because you are talking about objective patterns instead of subjective impressions.
When practices adopt this approach, surface electromyography becomes the motor lens through which you evaluate energy usage and coordination. It supports care plan conversations that feel logical and grounded. It also strengthens retention because patients can see progress. That is the heart of neurological scanning. It keeps the conversation focused on nervous system performance rather than only symptom control.
In research language you may see phrases like use of surface, based on surface, used in surface, surface EMG based, and even estimation of surface activity. In the clinic, the idea is simpler: repeatable scans help you evaluate whether the motor system is becoming more efficient under care.
INSiGHT neuroCORE and the Role of Surface Electromyography in Modern Chiropractic
For surface electromyography to work in a real chiropractic office, it has to be reproducible, practical, and easy to communicate. That is exactly where INSiGHT scanning technology fits. INSiGHT neuroCORE is the surface electromyography component of the INSiGHT neuroTECH ecosystem. It is designed for chiropractic SEMG scanning of paraspinal motor activity so doctors can collect objective exam data and compare recordings across time. The scan is fast, comfortable, and built for consistent use, which is what allows a chiropractor to track trends rather than rely on one-time impressions.
INSiGHT scanning technology does not create care plans. It produces objective scan results and reports. The chiropractor interprets that data and designs the care plan. INSiGHT software powered by Synapse supports that workflow by translating EMG signals into scan visuals that patients can quickly understand. Practically, it functions like a multi-channel surface approach, gathering multiple data points along the spine rather than a single reading. In that context, multi-channel surface electromyography helps you see distribution and symmetry patterns that matter clinically. It also helps you communicate why care is focused on neurological function, not just on a single sore region.
It is worth mentioning that the wider electromyography world includes many EMG applications beyond chiropractic, including lower limb EMG studies in sports and rehab, high-density surface EMG arrays in laboratories, and high-density surface electromyography mapping for research. You will also see terms like emg systems, signal processing, EMG signal processing, semg signal processing, systems and signal processing, and filtering of surface noise. Some research groups explore machine learning and classification of EMG signals, sometimes described as EMG classification, to sort movement patterns. Chiropractic does not need to become a lab. Chiropractic needs reliable data in the exam room. When the surface electromyography acquisition process is consistent, you can interpret patterns confidently and communicate them clearly.
From a scanning standpoint, the essentials still apply. Good signal acquisition means stable contact, consistent electrode placement, and a scan protocol that supports dependable recording. When that is in place, the raw EMG signal and even a raw EMG snapshot can be collected in a way that is clinically meaningful. The goal is not to overwhelm patients with technical talk. The goal is to show them how the nervous system is managing muscle force and stability, then use that clarity to support care decisions. That is the application of surface EMG in a neurologically focused practice, and it is why INSiGHT neuroCORE fits so naturally into a scan-centered workflow.
Where This Leads: A More Certain, More Understandable Chiropractic
Surface electromyography belongs in chiropractic because it makes the motor story visible. It helps you see how the nervous system is distributing tone, where neuromuscular coordination is efficient, and where compensation is costing the patient energy. It also gives you a reliable way to track change when symptoms fluctuate and stories get messy. When surface electromyography is used consistently, it strengthens the exam, the report of findings, and the long-term care plan conversation.
It is also a reminder of something chiropractors have always known. The body adapts. The nervous system organizes. When it cannot organize well, the motor system reveals it. SEMG gives you a window into that reality without needles and without guesswork. Even the basic distinctions matter: there are two kinds of EMG, and chiropractic surface EMG and intramuscular EMG are not interchangeable. Chiropractic SEMG is designed for repeatable scans, not disease diagnosis. That distinction keeps the conversation accurate, professional, and aligned with the purpose of neurological scanning.
If you want surface electromyography to have real impact in your practice, make it part of a scanning model, not a one-off event. Build baseline recordings, compare progress scans, and use the scan visuals to keep patients anchored to what matters: nervous system performance. And when you are ready to integrate this into a consistent exam rhythm, INSiGHT scanning technology, including INSiGHT neuroCORE and the INSiGHT software powered by Synapse, gives chiropractors a practical way to collect, interpret, and communicate surface EMG data with clarity. That is how scanning becomes more than technology. It becomes a language of certainty.
One final technical note for the chiropractors who like precision. The surface EMG signal you see is influenced by the surface area of detection, the tissue layers under the surface of the skin, and the quality of contact at the electrode surface. EMG signals are recorded through recording electrodes and an EMG sensor interface, producing surface electromyographic signals that can be evaluated through EMG signal analysis and analysis of EMG signals. That is the nature of the EMG. When you respect those fundamentals and keep your protocol consistent, you can confidently say that surface EMG changes reflect meaningful shifts in neuromuscular organization under care. That is working on EMG the right way in chiropractic, and it is how the use of surface electrodes supports better understanding, better communication, and better follow-through.