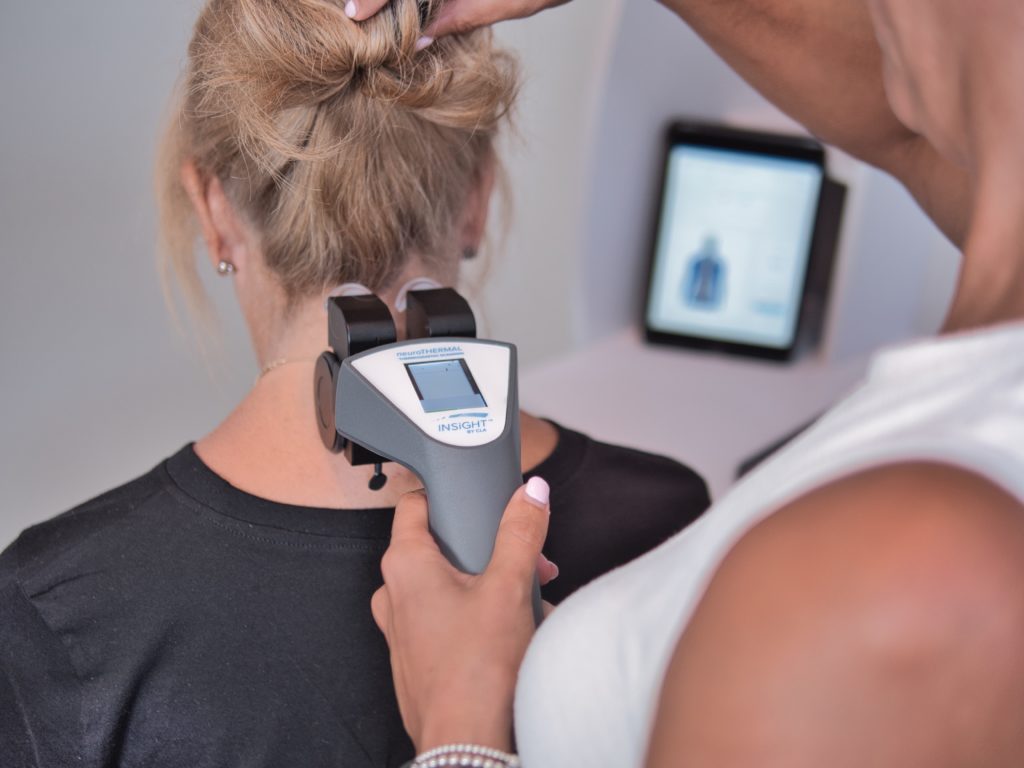
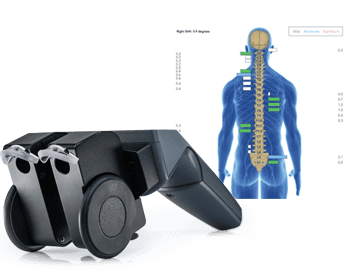
Because range of motion can change fast, ROM may look better after an adjustment, then tighten again after neurological distress, poor sleep, travel, or a long week. A joint can move more on Tuesday and less on Friday even when nothing structural has changed. That does not make range of movement less valuable. It means a range of motion assessment is a snapshot, not a diagnosis. The skill is knowing how to assess it, how to measure range of motion accurately, and how to interpret what it is really telling you.
Spinal ranges of motion are a window into how good the neuromotor performance is. If you are neurologically focused, there is a deeper layer. Joint movement is often the nervous system’s strategy on display. Protective tone, coordination, timing, and adaptability all influence the motion. That is why great chiropractors do not chase a number on a goniometer alone. They use a range of motion assessment as a doorway into better communication, better certainty, and better nervous system performance conversations.
Why Range of Motion Still Matters in Modern Chiropractic Patient Assessment
In chiropractic, range of motion is typically one of the first objective clues that function has shifted. When you do a range of motion assessment, you are measuring how far a joint can move through its arc of motion in a specific plane of motion, usually recorded in degrees. That might sound basic, but it matters. A clean range of motion assessment gives you a baseline that can be re-checked. It gives you assessment data that can be compared over time. It also helps you translate vague symptoms into something more concrete and less emotional.
Range of motion assessment also makes the musculoskeletal assessment feel real to a patient. They may not remember every orthopedic test, and they may not understand why you are asking about history and lifestyle. But they understand, “This joint range of motion is reduced compared to the other side,” or “This is your expected range, and right now you cannot access it.” In many clinics, ROM testing becomes part of the patient assessment because it gives the patient a shared reference point that is easy to see and easy to re-check. It is one reason range of motion testing is used so widely across chiropractic, physical therapy, and sports settings.
At the same time, we have to keep ROM in its proper lane. ROM is usually influenced by more than the joint itself. Guarding, fear, effort, and muscle strength can influence the motion. Neurological distress can influence the motion. Even the environment can influence the motion. That is why a range of motion assessment is most useful when it is consistent, and when it is paired with other objective information that helps you interpret why the range is limited or why it fluctuates.
- A range of motion assessment can highlight limited range of motion, but it rarely explains the whole cause.
- A range of motion assessment can show improvement, but it does not always prove stability.
- A range of motion assessment becomes more powerful when it is tracked alongside objective neurological trends.
That last point is the neurologically focused chiropractic advantage. A joint does not simply move because it has mechanical capacity. It moves because the nervous system allows it. That is why a range of motion assessment is not just about “mobility.” It is about how the nervous system is organizing limb motion, posture, and control. If you want the range of motion is usually meaningful, you have to read it in context.
Types of Range of Motion and What Each One Really Tells You
If you want your range of motion assessment to mean something, the first question is simple. What type of ROM are you looking at? In many clinics, ROM gets treated like one number. But in real practice, types of ROM are different conversations. The types of range of motion include active range of motion, passive range of motion, and active-assisted range of motion. Each one tells you something different about joint motion, control, and capacity.
Active range of motion is what the patient can do on their own. You will see it written as AROM, active ROM, or as part of an active ROM assessment. This is where you learn about coordination, willingness, and muscle strength expression. When you assess active ROM, do not only watch the angle. Watch the strategy. A patient may “find” shoulder flexion by arching the spine. A patient may “find” hip flexion by rolling the pelvis. If you do not control substitution, your ROM measurement becomes a mix of multiple regions instead of the motion of a joint you intended to test.
Passive range of motion is what you get when you move the joint for the patient. You may see it listed as PROM, passive motion, or a PROM assessment. Passive range of motion helps you estimate the structural capacity of the joint and surrounding non-contractile tissues. In many cases, passive range of motion is slightly greater than active range of motion. That is normal. But the comparison between active and passive is where the clinical insight lives. If passive motion is much greater than active motion, it can suggest inhibition, guarding, coordination issues, or a neurological component that is limiting access. Put simply, the joint may be capable, but the system is not granting access today. That is why a range of motion assessment is not just mechanical. It is neurological and mechanical working together.
Active-assisted range of motion sits in between. It is when the patient initiates movement and receives assistance to complete the movement. That might be your hands, a strap, a band, a dowel, or simple cueing. The assistance to complete the movement can reduce fear, reduce guarding, or improve organization. This is especially helpful when a patient has symptoms that spike near end range. Active-assisted range of motion can show you whether the system can access more joint ROM when the movement feels safer. It also helps you decide whether the limiter looks more like control, confidence, or a mechanical restriction.
One more key detail: end range is not only a number. It is also a feel. At the end of the ROM, the clinician notices the end-feel. A firm end-feel often suggests muscular or capsular tightness. A hard end-feel is more like bone meeting bone, which can be normal in certain motions. A soft end-feel can be normal when soft tissue compresses. An empty end-feel is when the patient stops you because symptoms show up before a true mechanical limit. This is why your range of motion assessment should always note the end of the ROM experience, not only the degrees.
ROM Testing Methods and Motion Measurement Tools That Hold Up in the Real World
ROM testing only becomes valuable when it becomes repeatable. Otherwise, you are collecting numbers that look objective but do not hold up when you re-check a week later, or when another clinician repeats the same range of motion assessment. That is why reliability and validity matter. They are the difference between a motion measurement you can build decisions on and a motion measurement that creates confusion. If you want a range of motion assessment to serve your care plan and documentation, treat standardization like part of the exam, not a side task.
The most common tool is still the goniometer. A goniometer is used to measure angles at a joint in degrees, and it is a workhorse in joint ROM assessment. Digital tools can help with readability and workflow, but the tool is not the magic. The method is. Whether you use a goniometer, a digital goniometer, or an inclinometer, your assessment methods should stay consistent. This is the core of reliability and validity of goniometric work. If you want the reliability and validity of goniometric data to improve inside your clinic, standardize who measures, how they measure, and how they document. That is how reliability and validity become practical, not theoretical.
Here is a simple process for conducting a ROM assessment that holds up in real life. Treat it as assessment before moving and handling, not a rushed add-on. Set the patient up the same way each time. Stabilize the segment you do not want moving. Move at a consistent speed. Watch for substitution. Then document the start and finish angles and whether you are testing active range of motion or passive range of motion. This process works whether you measure ROM by eye first and confirm with a tool, or you go straight to the instrument. It also respects that ROM may fluctuate for reasons that are not strictly mechanical.
- Preparation: position the patient consistently and, when appropriate, test the unaffected side first to establish expected range.
- Observation: watch the whole body for compensation and guarding, not just the joint movement.
- Stabilization: block the region you do not want contributing to the range of joint measurement.
- Alignment: use a goniometer with the axis aligned to the joint axis and the arms aligned with the long bones.
- Documentation: record angles and notes so your range of motion measurement can be repeated.
Clinics often ask which measurement tools are best. The better question is, which tools can you use consistently. A goniometer is inexpensive and reliable when used correctly. Inclinometers can be used to measure range when gravity-based angles are more practical. Digital devices can reduce reading errors. Apps and camera-based systems are emerging. But the goal stays the same: accurate assessment. The instrument is used to measure, but the clinician’s consistency is what makes it meaningful. That is also why it is worth teaching staff the same language and the same landmarks, so your range of motion and manual tracking is consistent visit to visit.
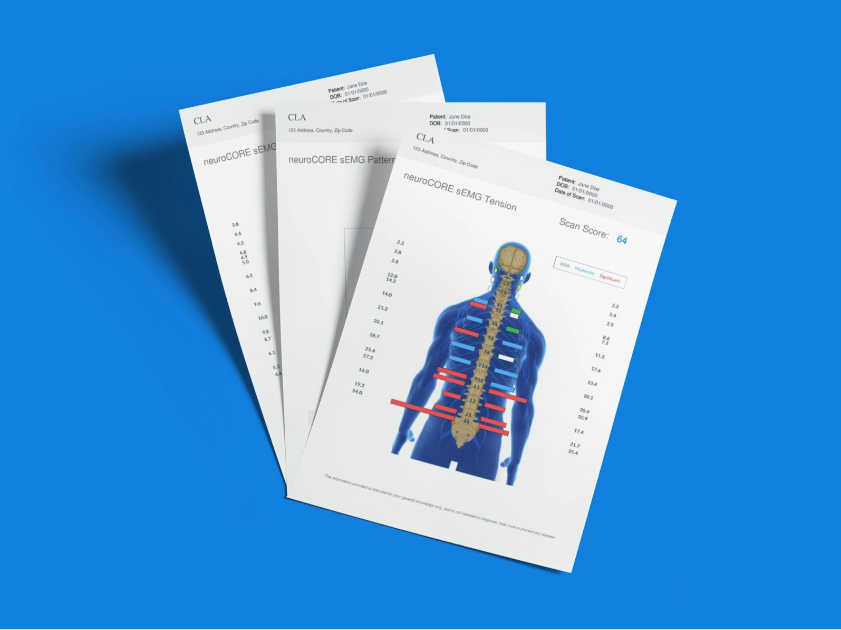
How INSiGHT Scanning Technology Adds More Meaning to a Range of Motion Assessment
A range of motion assessment tells you something important. It shows what the joint can do today. But for many patients, that finding is only one part of the story.
A shoulder may move better after an adjustment. A hip may open up more after a few visits. An ankle may suddenly access motion that was not there the week before. Those changes matter. But range of motion alone does not always explain why the motion improved, why it tightened back up, or why one patient holds their gains while another fluctuates.
That is where INSiGHT scanning technology becomes so valuable.
INSiGHT does not replace a range of motion assessment, and it does not replace your clinical judgment. It adds objective neurological exam data that helps you interpret the bigger picture. While ROM shows what is happening at the joint, INSiGHT helps you look deeper at nervous system performance, adaptation, and postural tension patterns that may be influencing that motion.
For example, neuroCORE sEMG can help you analyze patterns of postural tension and energy output that often show up alongside restricted or compensatory movement. neuroTHERMAL can help you observe regional stress trends that may relate to guarding and altered motor control. neuroPULSE HRV adds insight into adaptability and resilience, which matters because a patient in sympathetic overdrive often does not access movement the same way as a patient with better reserve.
That combination changes the conversation.
Instead of saying, “Your shoulder is tight,” you can say, “Your range of motion is reduced, and we are also seeing objective signs that your nervous system is under strain and not adapting well.” That creates more certainty for the chiropractor and more clarity for the patient. It also makes re-exams more meaningful, because now you are not only re-checking movement. You are re-checking whether the underlying neurological trends are moving in the right direction too.
This is one of the greatest strengths of INSiGHT scanning technology. It helps bridge the gap between what you see in motion and what may be driving that motion. Patients understand joint restriction. But when they also see scan views that reflect how their nervous system is adapting, the value of care becomes easier to explain and easier to retain.
A range of motion assessment gives you a functional snapshot. INSiGHT scanning technology gives you deeper context. Put them together, and your exam becomes more objective, your communication becomes stronger, and your care plan becomes easier to guide with confidence.
From ROM Numbers to Care Plan Clarity Using INSiGHT Scanning Technology For Interpretation and Communication
A common problem chiropractors face with their ROM testing is that numbers may improve quickly, then slide right back when life tightens the system again. That does not mean your care was wrong, it means the motion is typically performed under the influence of the nervous system’s protective strategy. That is why the best clinics treat ROM testing as one layer of assessment data, not the only one.
Range of motion testing can tell you what the joint can access today, but it does not always tell you why it is limited, why it improved, or whether the change will hold. If you want your range of motion assessment to guide a care plan with confidence, it needs context.
This is where INSiGHT scanning technology strengthens interpretation. It does not replace a goniometer and it does not replace motion measurement tools. It adds an objective neurological anchor to the patient assessment. neuroTHERMAL helps you observe segmental stress trends that often align with guarding and compensation. neuroCORE sEMG provides objective insight into motor tone and energy output trends that relate to stabilization strategies and how muscle strength expresses under load. neuroPULSE HRV adds adaptability and resilience context, which matters because stress physiology can influence the motion before a patient recognizes it. The INSiGHT does not produce a care plan. It generates objective exam data and reports that support the chiropractor’s interpretation, so the chiropractor can create a care plan that is more defensible and easier to communicate.
- ROM assessment using a goniometer shows what is happening locally in the joint range of motion today.
- INSiGHT scanning technology shows what is trending in nervous system performance that can influence the motion.
- When you re-check both, your ROM assessment becomes clearer and your progress conversation becomes calmer.
Practically, this is a simple workflow. Start with a baseline range of motion assessment and a baseline scan set. Then re-check key findings at logical intervals. This allows you to discuss change without over-explaining. You can say, “Your ROM measurement improved, and that is encouraging. Now let’s look at the neurological trend that helps us understand whether this improvement will hold.” In physical therapy and rehabilitation, ROM is assessed during a physical therapy intake and repeated often because it gives objective checkpoints. Chiropractic can do the same, while also tracking nervous system performance trends. That is how you move from isolated motion measurement to a care plan conversation built on objective clarity.
There are also situations where ROM goals look different, and your range of motion assessment should reflect that reality. After certain procedures, clinicians may use continuous passive motion in early stages to support knee motion goals. In more complex shoulder cases such as reverse total shoulder arthroplasty, the goal may be a stable, usable range, not a perfect number. This is why the best assessment typically includes multiple reference points. You still use a goniometer, you still measure ROM, and you still document changes. But you also build context around why the motion fluctuates and what influences the motion. When you combine ROM assessment using consistent methods with INSiGHT scanning technology, the story becomes clearer for you and for the patient.
A Clearer Way to Track Progress Without Guessing
A range of motion assessment can be one of the most practical tools in your clinic when you treat it with respect. Measure range of motion consistently. Know whether you are looking at active range of motion, passive range of motion, or active-assisted range of motion. Compare active and passive, and note what happens at end range. Use the same assessment methods so your numbers hold up. If you want to measure ROM well, keep your approach simple, repeatable, and honest.
Then put ROM where it belongs, inside a bigger clinical picture. Range of motion assessment is valuable, but it is not the whole story. A goniometer is used to measure joint angles, but it cannot explain why ROM may fluctuate or why a patient cannot access motion that seems mechanically available. That is where INSiGHT scanning technology strengthens certainty. It provides objective neurological context that supports communication, supports re-checks, and supports better care plan clarity. ROM tells you what the joint is doing today. INSiGHT helps you interpret what the nervous system is trending toward. When you bring those together, your range of motion assessment becomes more than a number. It becomes direction.